
Articles by Bangladesh

Improving the quality and availability of post-abortion care in a humanitarian crisis
The world is facing stronger and longer natural disasters, protracted complex emergencies, conflicts and epidemics. These humanitarian crises can expose weakness in health systems, with particularly serious consequences for women and girls in need of reproductive health care. To improve the quality and availability of post‑abortion care during a flood, the University of Leicester and International Planned Parenthood Federation South Asia Region (IPPF-SAR), in collaboration with the Government of Bangladesh, developed and measured the impact of an integrated intervention package, called RHCC. First tested in a flood-prone area of Bangladesh, this novel approach includes: i) Pre-positioning medicines and supplies, using the UNFPA’s Inter-Agency Reproductive Health Kit 8; ii) Capacity building of service providers; and iii) Community awareness raising. Supported by IPPF's Innovation Programme, the project aligns with IPPF’s commitment to ensuring that crisis-affected populations receive timely, quality, life-saving, gender-responsive and inclusive sexual and reproductive health services.

"...now I can provide MR (menstrual regulation) services efficiently."
Menstrual regulation, the method of establishing non-pregnancy for a woman at risk of unintended pregnancy, has been a part of Bangladesh’s family planning program since 1979. It is allowed up to 10 –12 weeks after a woman’s last menstrual period. Nursing Supervisor Ms. Lovely Yasmin is one of several staff members providing family planning, menstrual regulation, and post-procedure care services at Upzila Health Complex in Belkuchi, Bangladesh. “Before this training we used to sometimes advise people on such services and provided menstrual regulation (MR) services but after the training I’ve have become and confident and efficient in providing MR services,” she says. “Earlier there could possibly have been mistake but now I can provide MR services efficiently and perfectly. I can now provide MR services in more organized manner.” But while Yasmin, who has worked in family planning for 16 years, says that the recent training has increased her confidence in properly doing MR procedures, the health complex still lacks basic supplies. “There were difficulties due to limited equipment,” she says. “We sometimes have to use personal equipment.” But, she says, the presence of Kit 8 has made life easier. “Prior to this kit, many clients did not complete the full course of medical as advices due to financial issues… during floods there are many hardships including financial difficulty,” she says. “However with this kit, most of the medicines are provided and clients are easily managing on their own.”
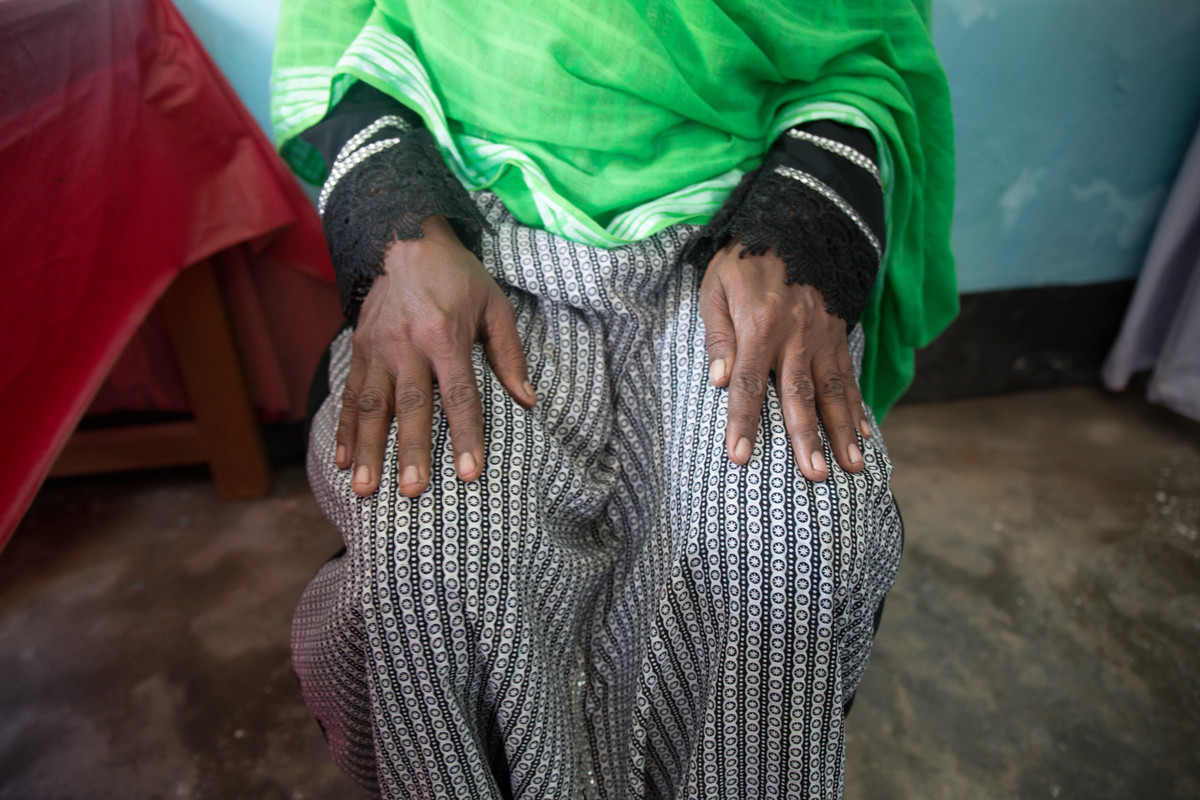
“After the menstrual regulations services I was prescribed a few medicines which I could not buy due to poor financial condition”
Menstrual regulation, the method of establishing non-pregnancy for a woman at risk of unintended pregnancy, has been a part of Bangladesh’s family planning program since 1979. It is allowed up to 10 –12 weeks after a woman’s last menstrual period. When Shana Khatun, a mother of three, became pregnant again she says she began to feel very weak and had issues with massive bleeding.Citing her age and the possibility of further medical complications, Khatun decided to undergo a menstrual regulation procedure. “But if the hospital and services weren’t there then I would have had to have continued with my pregnancy, even when (I do) not want another child” she says. Khatun says that the procedure went well, but that without the presence of medicine found in Kit 8 she would have lacked post-operation medicine. “After the menstrual regulations services I was prescribed a few medicines which I could not buy due to poor financial condition,” she says. “But the hospital gave me a number of medicines that I could take.” And while Khatun had talked with women about various family planning methods, she didn’t feel she could talk with anyone aside from her husband about getting the procedure. “I feared they would treat me poorly (the hospital),” she says. But Kahtun says she found the hospital trustworthy and helpful, even when she was suffering complications such as mass bleeding. “I will be very cautious that I should not get pregnant again however in event if I get pregnant again then I will come to this hospital only,” she says.

Small scale innovation in Bangladesh during times of crisis: ensuring reproductive care to local communities
In times of humanitarian crises and disasters, the inability to access health care during floods can have serious repercussions on the local community. As part of their Innovation Programme project, our South Asia office in collaboration with the University of Leicester and the Government of Bangladesh provides reproductive health kits to health centres located in areas most prone to seasonal flooding. Known as 'Kit 8' it contains three months’ worth of medicine and equipment for the management of miscarriage and complications of abortion and menstrual regulation in emergency situations, essential to minimize associated morbidity and mortality. Medical staff are trained to administer procedures and provide post-procedure care. While abortion is considered illegal in Bangladesh, menstrual regulation, which has been a part of the country’s family planning program since 1979, is allowed up to 10–12 weeks after a woman’s last menstrual period. Photography © IPPF/Victoria Milko

“My spouse was supportive and he gave me the freedom to come to this decision myself”
Menstrual regulation, the method of establishing non-pregnancy for a woman at risk of unintended pregnancy, has been a part of Bangladesh’s family planning program since 1979. It is allowed up to 10 –12 weeks after a woman’s last menstrual period. Auliya Khatun, a mother of three children, was 40 years old when she found out that she had unintentionally become pregnant again. Khatun says she had heard about family planning services and menstrual regulation services available at the Upzila Health Complex from other women in her small village. She discussed the option of undergoing menstrual regulation with her husband. “My spouse was supportive and he gave me the freedom to come to this decision myself,” Khatun says. “If this service was not available then I would have carried on with the pregnancy. It would have been embarrassing, though,” she explains. “It is embarrassing to have another child at this age.” Khatun, who sometimes assists her husband with work in a local handloom, also cited the financial burden another child would have on her family. “We are facing financial difficulty so it is not possible to have another child.” Khatun says she only experienced mild gastric discomfort after the procedure but felt assured about her recovery due to being able to check-in with doctors at the local health centre. The access to the services and doctors, she says, was a major factor in a smooth and easy recovery. “Since this service was in a government facility I could prevail [through] this and survive,” she says. “It is an important service.”

Ensuring women and girls receive healthcare during humanitarian crises in Bangladesh
In Bangladesh menstrual regulation, the method of establishing non-pregnancy for a woman at risk of unintended pregnancy, has been a part of the country’s family planning program since 1979 and is allowed up to 10 –12 weeks after a woman’s last menstrual period. There are no legal restrictions on providing post-abortion care. Dhukuriabera Family Health & Welfare Centre is prone to flooding during rainy season in Bangladesh. The watermarks on the walls of the clinic from last year’s flood almost reach the ceiling, and serve as a reminder of the extreme circumstances staff at the centre face in providing vital healthcare during a humanitarian crisis. “Our office was flooded. We had to stand on chairs,” says Salma Parvin, a staff member of the centre, pointing to mildew marks on the walls. “Very few patients came to access services.” “During floods there are lots of challenges,” says Dr. Laila Arjumand Banu at the Belkuchi Upazila Health & Family Planning Complex. “People get stuck and may forget to use the normal family planning methods.” The inability to access medical centres during floods can have other repercussions. “[When there are floods] clients sometimes have a procedure done by a village provider and thereafter come to us with complications,” says nursing supervisor Lovely Yasmin. “And then we have to provide services with [medical equipment] that we don’t have.” As part of their Innovation Programme project, IPPF’s South Asia office the IPPF South Asia office in collaboration with the University of Leicester and the Government of Bangladesh have has begun distributing UNFPA’s reproductive health kit 8 in strategic locations most prone to seasonal flooding. Kit 8 contains three months’ worth of medicine and equipment for the management of miscarriage and complications of unsafe abortion in emergency situations, essential to minimize associated morbidity and mortality. “I find the kits very useful,” says nurse Lipara Khatun. “Patients will benefit as they can avail these services closer to home and not have to come all the way to centres.” At her home in the village of Charmokimpur, Bijli Khatun, 32, explains how flooding was just one of many challenges her unplanned pregnancy presented. “One of [my] children is disabled and so the fear of possibly another disabled child was scary,” Bijli Khatun says. “And during the pregnancy I felt a lot of pain in my stomach and decided to get menstrual regulation.” Bijli Khatun’s husband had heard about menstrual regulation services at the local health centre. Bijli decided she would undergo the procedure, but soon realized she would face some issues. “The area surrounding my house was submerged in water,” she explains. “With great difficulty I went to the centre and it was closed that day so I had to come back and once the water receded then I went to the centre again and got a menstrual regulation procedure done.” Even with legal validity, social stigma is another factor women have to consider. “Women who come are hesitant and do not share their health problem easily,” says nurse Lovely Yasmin. “They expect complete confidentiality… as people are religious and [the woman] might have problems at home or in her locality.” The programme also provides vital post-procedure care –most commonly pain relief- of which many women who undergo menstrual regulation, would be unable to afford themselves. Shana Khatun, 34 says “After the menstrual regulation services the hospital gave me a number of medicines I could take, I was also prescribed a few medicines which I could not buy due to [my] poor financial condition.” Shubhutara is another client. She’s 32 and a mother of four, and decided to undergo menstrual regulation services after finding out she was pregnant again. “Even though I have [undergone] menstrual regulation I would not want to tell others,” she says. “They will feel I have sinned and they will insult me.” Several of the women feared being identified by the community, saying they would face a backlash due to conservative religious beliefs held in the region. Shana Khatun says she found the hospital trustworthy and helpful. “I will be very cautious that I should not get pregnant again,” she says. “However in the event I get pregnant again, then I will come to this hospital only.” IPPF’s Innovation Programme supports small scale initiatives, which test new ways to tackle the biggest challenges in sexual and reproductive health and rights. Each project is partnered with a research organization, in this case the University of Leicester, to ensure their impact is measured and learning shared to improve the efficacy and evidence-base of our programming.
IPPF responds to the Rohingya crisis
One of the worst refugee crises in recent years has been that facing the Rohingya. Thousands have fled their homes in Myanmar following a horrific campaign of violence which started in August 2017. Over 600,000 Rohingya sought refuge in Bangladesh, and the majority are still living in camps there until it is safe enough to return. As with any crisis situation, the provision of sexual and reproductive healthcare is essential, and IPPF clinics and local organizations on the ground have helped ensure that these needs do not go unmet. Rehana’s story We spoke to 25-year-old Rehana Begum who is 8 months pregnant with three small children in tow. She was one of the hundreds of thousands forced to leave home amidst the crisis. Heavily pregnant and exhausted, her and her family walked for 15 days to reach safety in Bangladesh. Rehana visited an IPPF health clinic for a check-up and was provided with antenatal care. This was the first time during any of her pregnancies that she has had any medical attention. Before attending the clinic Rehana was unaware of family planning as a way to plan future pregnancies. “I was not aware of family planning methods earlier,” she told us. “I am happy to know that I have options in terms of controlling my family size. I would definitely want to adopt a family planning method after my delivery”. Delivering essential healthcare Working with local organizations, IPPF’s focus is on delivering sexual and reproductive healthcare to the camp. Women and girls make up 94% of clinic visits, with 77% of total visitors who received sexual healthcare under 25-years-old. Field teams have been mobilized to create awareness about sexually transmitted diseases and birth control methods. IPPF has partnered with various local agencies for provision of these services as well as distribution of the kits and medical supplies.

Bangladesh’s new Child Marriage Act is a step backwards for young women warns IPPF
New legislation in Bangladesh which will allow girls under the age of 18 to be married-off legally in “special circumstances” is a step backwards for young woman, the International Planned Parenthood Federation has warned. The Child Marriage restraint Bill 2017 gives parents or guardians the ability to seek a court order for children to be married-off in their “best interests.” Currently, it is illegal for girls under 18 or men under 21 to marry in Bangladesh, although the law is widely flouted. The new law opens the possibility of girls who have been raped being married to their attackers or girls who have become pregnant being married to abusers. Anjali Sen, regional director for IPPF’s South Asia Region, which includes Bangladesh, said the new legislation was a move in the wrong direction. “Any legislation which opens the possibility of young girls being forced into marriage is going the wrong way,” she said. “Countries around the world and in the South Asia region are looking to close loopholes around child marriage and tighten restrictions, rather than create new exceptions which allow it. “We know that early marriage for young girls is likely to lead to them dropping out of school and narrows their life chances. “This new legislation appears to work against Bangladesh’s welcome commitment to ending child marriage – which means marriage before 18 – by 2041 and reducing it by a third by 2021. “IPPF would urge the Government of Bangladesh to think again about this legislation and the rights of the young girls it threatens to undermine.” Bangladesh has one of the highest rates of child marriage in the world, according to a 2016 UNICEF report, which said 52% of girls in Bangladesh were married before the age of 18 and nearly 20% by 15. IPPF is a global federation of locally-owned associations and partners providing and campaigning for sexual and reproductive health care and rights in 170 countries.
Girls Decide
This programme addresses critical challenges faced by young women around sexual health and sexuality. It has produced a range of advocacy, education and informational materials to support research, awareness-raising, advocacy and service delivery. Girls Decide is about the sexual and reproductive health and rights of girls and young women. Around the world, girls aged 10 to 19 account for 23% of all disease associated with pregnancy and childbirth. An estimated 2.5 million have unsafe abortions every year. Worldwide, young women account for 60% of the 5.5 million young people living with HIV and/or AIDS. Girls Decide has produced a range of advocacy, education and informational materials to support work to improve sexual health and rights for girls and young women. These include a series of films on sexual and reproductive health decisions faced by 6 young women in 6 different countries. The films won the prestigious International Video and Communications Award (IVCA). When girls and young women have access to critical lifesaving services and information, and when they are able to make meaningful choices about their life path, they are empowered. Their quality of life improves, as does the well-being of their families and the communities in which they live. Their collective ability to achieve internationally agreed development goals is strengthened. Almost all IPPF Member Associations provide services to young people and 1 in every 3 clients is a young person below the age of 25. All young women and girls are rights-holders and are entitled to sexual and reproductive rights. As a matter of principle, the IPPF Secretariat and Member Associations stand by girls by respecting and fulfilling their right to high quality services; they stand up for girls by supporting them in making their own decisions related to sexuality and pregnancy; they stand for sexual and reproductive rights by addressing the challenges faced by young women and girls at local, national and international levels.







