Spotlight
A selection of stories from across the Federation

France, Germany, Poland, United Kingdom, United States, Colombia, India, Tunisia
Abortion Rights: Latest Decisions and Developments around the World
The global landscape of abortion rights continues to evolve in 2024, with new legislation and feminist movements fighting for better access. Let's take a trip around the world to see the latest developments.
Most Popular This Week
France, Germany, Poland, United Kingdom, United States, Colombia, India, Tunisia

Abortion Rights: Latest Decisions and Developments around the World
Over the past 30 years, more than

Palestine

In their own words: The people providing sexual and reproductive health care under bombardment in Gaza
Week after week, heavy Israeli bombardment from air, land, and sea, has continued across most of the Gaza Strip.
Vanuatu

When getting to the hospital is difficult, Vanuatu mobile outreach can save lives
In the mountains of Kumera on Tanna Island, Vanuatu, the village women of Kamahaul normally spend over 10,000 Vatu ($83 USD) to travel to the nearest hospital.
Vanuatu

Sex: changing minds and winning hearts in Tanna, Vanuatu
“Very traditional.” These two words are often used to describe the people of Tanna in Vanuatu, one of the most populated islands in the small country in the Pacific.
Vanuatu

Vanuatu cyclone response: The mental health toll on humanitarian providers
Girls and women from nearby villages flock to mobile health clinics set up by the Vanuatu Family Health Association (VFHA).
Cook Islands

Trans & Proud: Being Transgender in the Cook Islands
It’s a scene like many others around the world: a loving family pour over childhood photos, giggling and reminiscing about the memories.
Cook Islands

In Pictures: The activists who helped win LGBTI+ rights in the Cook Islands
The Cook Islands has removed a law that criminalizes homosexuality, in a huge victory for the local LGBTI+ community.
Filter our stories by:
- Albanian Center for Population and Development
- Association Malienne pour la Protection et la Promotion de la Famille
- Family Guidance Association of Ethiopia
- Family Planning Association of Nepal
- Palestinian Family Planning and Protection Association (PFPPA)
- Planned Parenthood Federation of Nigeria
- Reproductive & Family Health Association of Fiji
- Reproductive Health Association of Cambodia (RHAC)
- Reproductive Health Uganda
- Somaliland Family Health Association
- Tonga Family Health Association
- Vanuatu Family Health Association


| 18 December 2018
"Many of the women we work with have no health insurance"
Hatixhe Gorenca is a nurse at the Albanian Centre of Population and Development (ACPD) clinic in Tirana. She joined the center in 2013 with 39 years of experience working in gynaecology. During her time as a nurse, she has seen vast improvements in access and services for cervical cancer screenings. However, she says that there is a considerable number of women in rural areas that face difficulties in accessing healthcare, and some that cannot access it at all. Rural women & access “The ACPD clinic is crucial for these [rural] women, because the healthcare we offer through gynaecological visits, includes counselling, pap smears, colposcopies and recently VIA tests and cryotherapy. Services that are totally missing in their areas. What they appreciate most is the mobile clinic in the outskirts of Tirana, because they have an opportunity to meet with doctors and to get information about their health status. We do approximately 17-18 visits per day and the number is always increasing”, Hatixhe says. The clinic has developed a reputation for offering youth-friendly healthcare and information. The confidential and open approach of the clinic is providing access for girls to comprehensive sexual education at an early age, without fear of discrimination or embarrassment. When the clinic first introduced VIA testing in 2017, as an alternative way for the screening of cervical cancer, it was welcomed by the women. “The reason is that compared to pap smears, VIA gives an immediate response on the health of the cervical cells,” Hatixhe explains. “The other reason is economical. Many of the women we work with have no health insurance, as such they cannot benefit from the free tests at maternity hospitals. Furthermore, some of them are vulnerable women and they feel safe when they can get free information and healthcare at our clinic.” What is VIA & Cryotherapy? Show more + Visual inspection of the cervix with acetic acid (VIA) is a process of screening and examining the cervix. Pre-cancerous lesions on the cervix will turn white when the acid is applied. This simple procedure can be done in a clinic setting without the use of a laboratory and allows for immediate treatment of any pre-cancerous lesions with cryotherapy. Cryotherapy is a gynaecological treatment that freezes and destroys abnormal, pre-cancerous cervical cells. Cryotherapy is not a treatment for cervical cancer. VIA has the potential to revolutionize cervical cancer prevention efforts, particularly in low resource settings, because it eliminates the need for laboratories, transportation of specimens and provides immediate test results. VIA needs less equipment and fewer specialists than traditional cervical cancer screening methods like Pap smears. Results from VIA are available immediately so women can be screened and treated in one single visit. ACDP outreach activities enable the staff to give the information where the women are: in the streets, in their workplace, in their homes. Hatixhe has witnessed a growing interest in women regarding their reproductive health in recent years. The number of women that walk through the clinic doors is proof of that. During the 2016-2017 over 3,000 women received healthcare services from the clinic. Encouraging other women “I myself am learning a lot in the clinic”, Hatixhe says. “VIA test was a new technique even for me, but it is so simple, I can now train the staff at the health centers. I can tell you that they are very enthusiastic and responsive because VIA is very easy to apply. Since many health centers have no gynaecological bed for their visits or low capacities to apply PAP tests which require specialized personnel, VIA is much more suitable for their conditions, because it can be done by the nurses or midwifes themselves.” Hatixhe is impressed by the reaction of women taking VIA tests. “As a nurse with long experience in the health sector, I have received many thanks from patients, but the hugs we get from these women are heartfelt. After 2-3 years of coming and going to different institutions, finally, they have found a method which can detect pre-cancer cells, get treatment for it and now they are totally healthy.” Hatixhe says that many women have been encouraged to book a VIA test through hearing about it from a friend or relative who had a positive experience at the clinic. “After the first visit, the women return with other women who are interested to do the tests. This is wonderful.”

| 19 April 2024
"Many of the women we work with have no health insurance"
Hatixhe Gorenca is a nurse at the Albanian Centre of Population and Development (ACPD) clinic in Tirana. She joined the center in 2013 with 39 years of experience working in gynaecology. During her time as a nurse, she has seen vast improvements in access and services for cervical cancer screenings. However, she says that there is a considerable number of women in rural areas that face difficulties in accessing healthcare, and some that cannot access it at all. Rural women & access “The ACPD clinic is crucial for these [rural] women, because the healthcare we offer through gynaecological visits, includes counselling, pap smears, colposcopies and recently VIA tests and cryotherapy. Services that are totally missing in their areas. What they appreciate most is the mobile clinic in the outskirts of Tirana, because they have an opportunity to meet with doctors and to get information about their health status. We do approximately 17-18 visits per day and the number is always increasing”, Hatixhe says. The clinic has developed a reputation for offering youth-friendly healthcare and information. The confidential and open approach of the clinic is providing access for girls to comprehensive sexual education at an early age, without fear of discrimination or embarrassment. When the clinic first introduced VIA testing in 2017, as an alternative way for the screening of cervical cancer, it was welcomed by the women. “The reason is that compared to pap smears, VIA gives an immediate response on the health of the cervical cells,” Hatixhe explains. “The other reason is economical. Many of the women we work with have no health insurance, as such they cannot benefit from the free tests at maternity hospitals. Furthermore, some of them are vulnerable women and they feel safe when they can get free information and healthcare at our clinic.” What is VIA & Cryotherapy? Show more + Visual inspection of the cervix with acetic acid (VIA) is a process of screening and examining the cervix. Pre-cancerous lesions on the cervix will turn white when the acid is applied. This simple procedure can be done in a clinic setting without the use of a laboratory and allows for immediate treatment of any pre-cancerous lesions with cryotherapy. Cryotherapy is a gynaecological treatment that freezes and destroys abnormal, pre-cancerous cervical cells. Cryotherapy is not a treatment for cervical cancer. VIA has the potential to revolutionize cervical cancer prevention efforts, particularly in low resource settings, because it eliminates the need for laboratories, transportation of specimens and provides immediate test results. VIA needs less equipment and fewer specialists than traditional cervical cancer screening methods like Pap smears. Results from VIA are available immediately so women can be screened and treated in one single visit. ACDP outreach activities enable the staff to give the information where the women are: in the streets, in their workplace, in their homes. Hatixhe has witnessed a growing interest in women regarding their reproductive health in recent years. The number of women that walk through the clinic doors is proof of that. During the 2016-2017 over 3,000 women received healthcare services from the clinic. Encouraging other women “I myself am learning a lot in the clinic”, Hatixhe says. “VIA test was a new technique even for me, but it is so simple, I can now train the staff at the health centers. I can tell you that they are very enthusiastic and responsive because VIA is very easy to apply. Since many health centers have no gynaecological bed for their visits or low capacities to apply PAP tests which require specialized personnel, VIA is much more suitable for their conditions, because it can be done by the nurses or midwifes themselves.” Hatixhe is impressed by the reaction of women taking VIA tests. “As a nurse with long experience in the health sector, I have received many thanks from patients, but the hugs we get from these women are heartfelt. After 2-3 years of coming and going to different institutions, finally, they have found a method which can detect pre-cancer cells, get treatment for it and now they are totally healthy.” Hatixhe says that many women have been encouraged to book a VIA test through hearing about it from a friend or relative who had a positive experience at the clinic. “After the first visit, the women return with other women who are interested to do the tests. This is wonderful.”
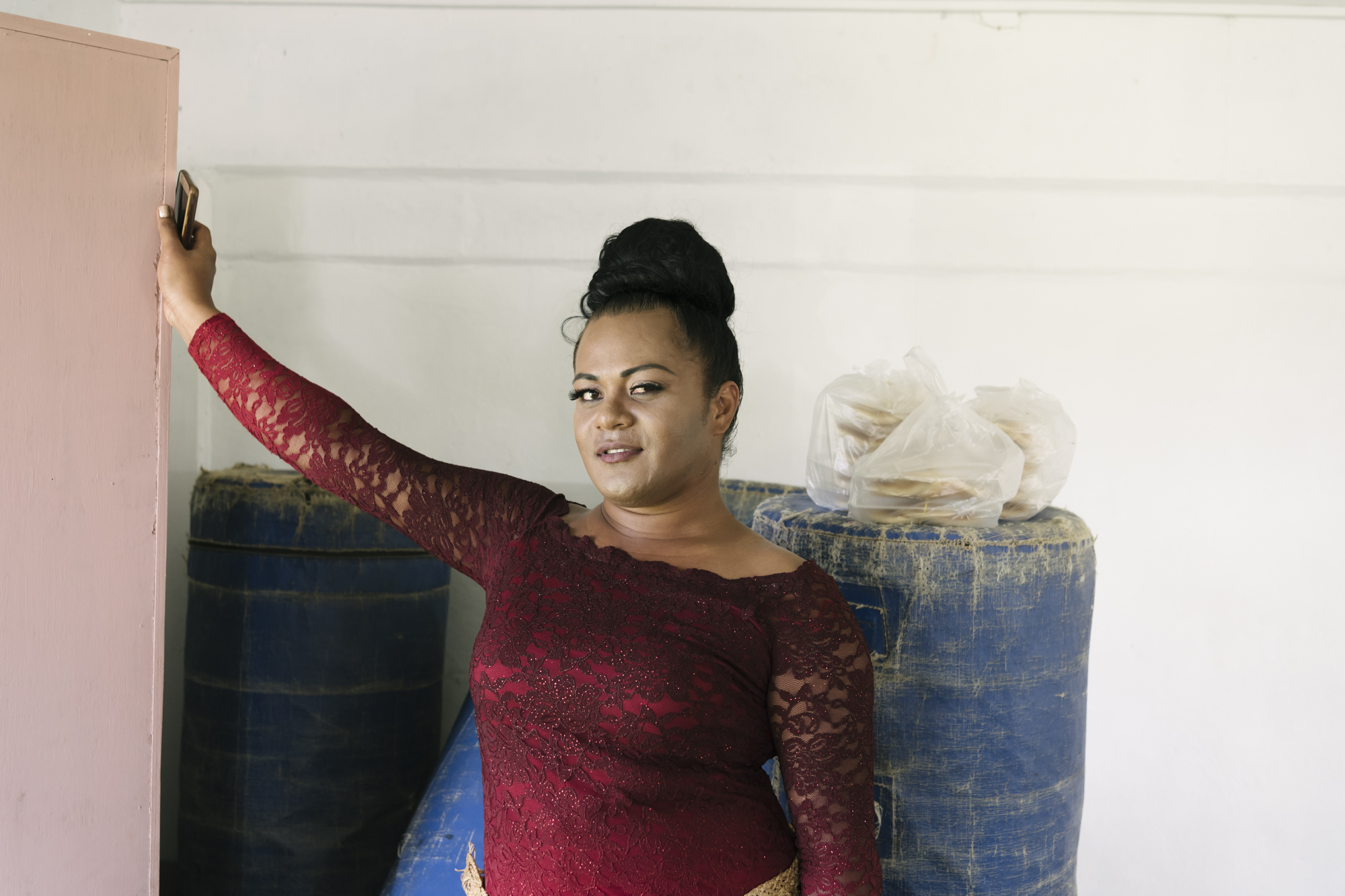
| 29 March 2018
"I have a feeling the future will be better"
Leiti is a Tongan word to describe transgender women, it comes from the English word “lady”. In Tonga the transgender community is organized by the Tonga Leiti Association (TLA), and with the support of Tonga Family Health Association (TFHA). Together they are educating people to help stop the discrimination and stigma surrounding the Leiti community. Leilani, who identifies as a leiti, has been working with the Tonga Leiti Association, supported by Tonga Health Family Association to battle the stigma surrounding the leiti and LGBTI+ community in Tonga. She says "I started to dress like a leiti at a very young age. Being a leiti in a Tongan family is very difficult because being a leiti or having a son who’s a leiti are considered shameful, so for the family (it) is very difficult to accept us. Many leitis run away from their families." Frequently facing abuse Access to health care and sexual and reproductive health service is another difficulty the leiti community face: going to public clinics, they often face abuse and are more likely to be ignored or dismissed by staff. When they are turned away from other clinics, Leilani knows she can always rely on Tonga Health Family Association for help. 'I think Tonga Family Health has done a lot up to now. They always come and do our annual HIV testing and they supply us (with) some condom because we do the condom distribution here in Tonga and if we have a case in our members or anybody come to our office we refer them to Tonga Family Health. They really, really help us a lot. They (are the) only one that can understand us." Tonga Family Health Association and Tonga Leiti Association partnership allows for both organisations to attend training workshops run by one another. A valuable opportunity not only for clinic staff but for volunteers like Leilani. "When the Tonga Family Health run the training they always ask some members from TLA to come and train with them and we do the same with them. When I give a presentation at the TFHA's clinic, I share with people what we do; I ask them for to change their mindset and how they look about us." Overcoming stigma and discrimination With her training, Leilani visits schools to help educate, inform and overcome the stigma and discrimination surrounding the leiti community. Many young leiti's drop out of school at an early age due to verbal, physical and in some cases sexual abuse. Slowly, Leilani is seeing a positive change in the schools she visits. “We go to school because there a lot of discrimination of the leiti's in high school and primary school too. I have been going from school to school for two years. My plan to visit all the schools in Tonga. We mostly go to all-boys schools is because discrimination in school is mostly done by boys. I was very happy last year when I went to a boys school and so how they really appreciate the work and how well they treated the Leiti's in the school." In February, Tonga was hit by tropical cyclone Gita, the worst cyclone to hit the island in over 60 years. Leilani worries that not enough is being done to ensure the needs of the Leiti and LGBTI+ community is being met during and post humanitarian disasters. "We are one of the vulnerable groups, after the cyclone Gita we should be one of the first priority for the government, or the hospital or any donations. Cause our life is very unique and we are easy to harm." Despite the hardships surrounding the leiti community, Leilani is hopeful for the future, "I can see a lot of families that now accept leiti's in their house and they treat them well. I have a feeling the future will be better. Please stop discriminating against us, but love us. We are here to stay, we are not here to chase away." Watch the Humanitarian teams response to Cyclone Gita
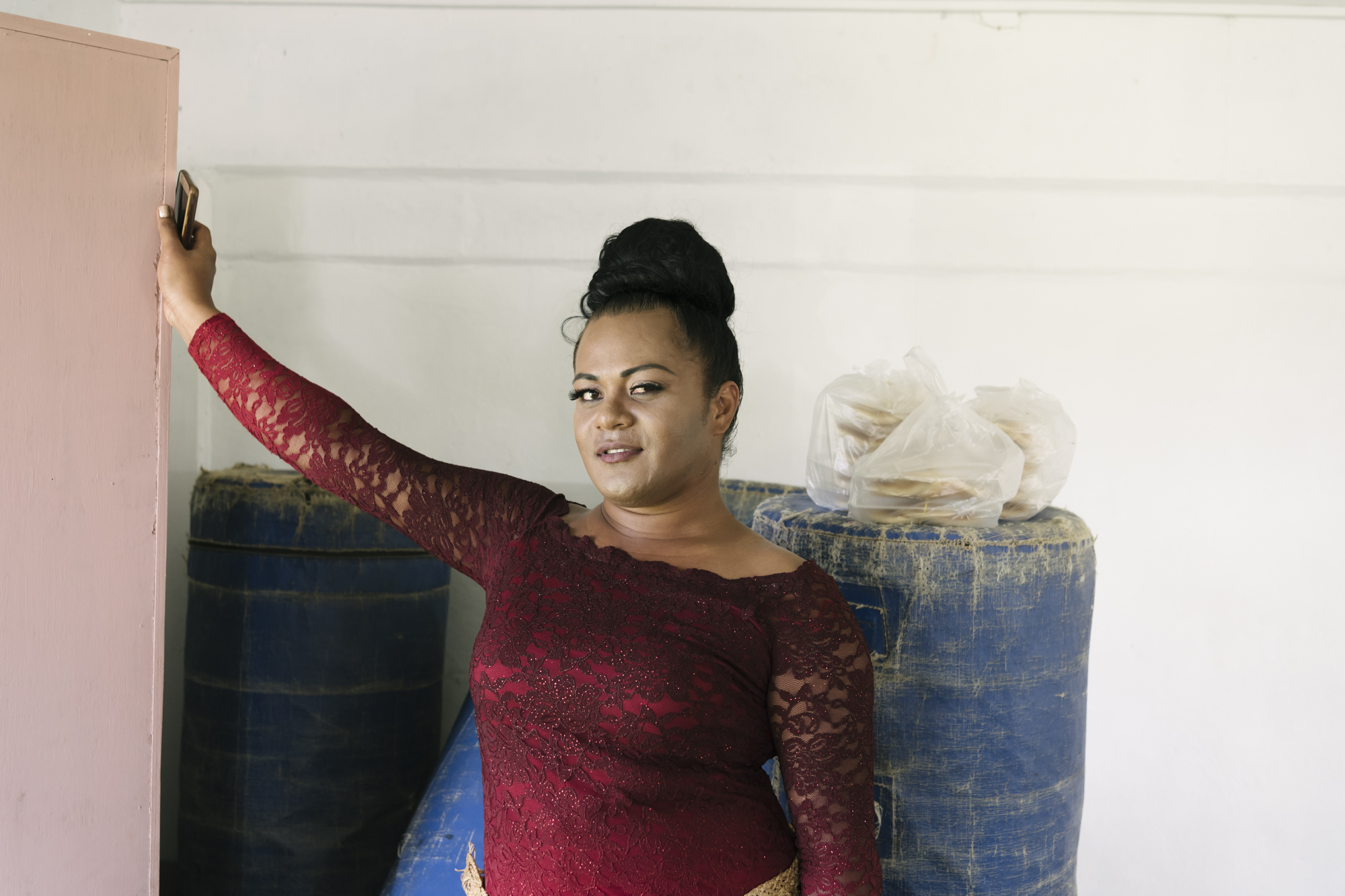
| 19 April 2024
"I have a feeling the future will be better"
Leiti is a Tongan word to describe transgender women, it comes from the English word “lady”. In Tonga the transgender community is organized by the Tonga Leiti Association (TLA), and with the support of Tonga Family Health Association (TFHA). Together they are educating people to help stop the discrimination and stigma surrounding the Leiti community. Leilani, who identifies as a leiti, has been working with the Tonga Leiti Association, supported by Tonga Health Family Association to battle the stigma surrounding the leiti and LGBTI+ community in Tonga. She says "I started to dress like a leiti at a very young age. Being a leiti in a Tongan family is very difficult because being a leiti or having a son who’s a leiti are considered shameful, so for the family (it) is very difficult to accept us. Many leitis run away from their families." Frequently facing abuse Access to health care and sexual and reproductive health service is another difficulty the leiti community face: going to public clinics, they often face abuse and are more likely to be ignored or dismissed by staff. When they are turned away from other clinics, Leilani knows she can always rely on Tonga Health Family Association for help. 'I think Tonga Family Health has done a lot up to now. They always come and do our annual HIV testing and they supply us (with) some condom because we do the condom distribution here in Tonga and if we have a case in our members or anybody come to our office we refer them to Tonga Family Health. They really, really help us a lot. They (are the) only one that can understand us." Tonga Family Health Association and Tonga Leiti Association partnership allows for both organisations to attend training workshops run by one another. A valuable opportunity not only for clinic staff but for volunteers like Leilani. "When the Tonga Family Health run the training they always ask some members from TLA to come and train with them and we do the same with them. When I give a presentation at the TFHA's clinic, I share with people what we do; I ask them for to change their mindset and how they look about us." Overcoming stigma and discrimination With her training, Leilani visits schools to help educate, inform and overcome the stigma and discrimination surrounding the leiti community. Many young leiti's drop out of school at an early age due to verbal, physical and in some cases sexual abuse. Slowly, Leilani is seeing a positive change in the schools she visits. “We go to school because there a lot of discrimination of the leiti's in high school and primary school too. I have been going from school to school for two years. My plan to visit all the schools in Tonga. We mostly go to all-boys schools is because discrimination in school is mostly done by boys. I was very happy last year when I went to a boys school and so how they really appreciate the work and how well they treated the Leiti's in the school." In February, Tonga was hit by tropical cyclone Gita, the worst cyclone to hit the island in over 60 years. Leilani worries that not enough is being done to ensure the needs of the Leiti and LGBTI+ community is being met during and post humanitarian disasters. "We are one of the vulnerable groups, after the cyclone Gita we should be one of the first priority for the government, or the hospital or any donations. Cause our life is very unique and we are easy to harm." Despite the hardships surrounding the leiti community, Leilani is hopeful for the future, "I can see a lot of families that now accept leiti's in their house and they treat them well. I have a feeling the future will be better. Please stop discriminating against us, but love us. We are here to stay, we are not here to chase away." Watch the Humanitarian teams response to Cyclone Gita

| 05 February 2018
"Dignity, respect and bravery are guiding principles for our work on female genital mutilation (FGM)"
I left Somaliland when I was 9 years old with my mother, brother, uncles, aunts and cousins. It was the civil war and we were lucky enough to reach Canada as refugees. I remember that time as a pleasant, warm, loving time where my cousins and I had a lot of freedom to play, walk to school and daydream. I am from Somaliland so of course I am part of the 97-98% or so of girls who undergo the female genital cut. I think it happened when I was around seven years old. I remember being restrained. I remember strangers being around and I remember peeing standing up and it burning. These memories don’t come up often and they don’t cause me pain. It’s a distant, childhood event. A cousin and a niece my age were there and we went through it together and afterwards our mothers and aunts took care of us. I grew up, went to school, questioned the world and my role in it for a time, got married, had kids and eventually went back to Somaliland. There I met Edna Adan Ismail and asked to volunteer with her. She opened her office, hospital and life to me and I became immersed in the maternal health issues of the women in my home country. The effort to end FGM Most were not as lucky as I had been. Because of FGM/C (female genital mutilation/circumcision), most had experienced recurring infections and difficulties in child birth. Some had formed cysts, some became infertile, and some had obstetric fistula. But few linked these problem to the cutting. At SOFHA (Somaliland Family Health Association) we’ve been working to help women (and men) understand these links and get the help they need. That’s only a part of the work. The effort to end FGM/C in Somaliland goes back almost 40 years. FGM/C programs and projects have been happening for at least the last 25 years. We’re now at the point where it’s recognized as a legitimate, critical, health and social issue. We’re on the cusp of a law against the practice and I have personally witnessed a transformation among the individuals who engage in this work. NGO and government staff tasked with working on FGM/C used to go into communities apologetically, “Sorry but we have to talk to you about this ‘issue’, we know it’s unpleasant but bear with us” to “I have 2 daughters and I have not cut them. This is a terrible practice and we must stop it now”. It fills me with great joy to see young women and men taking this personal stance and doing it confidently and proudly. But it’s not easy for most people to do this. It certainly wasn’t for me. This is personal. This is private. Before I got into the work I might have said, “What business is it of yours anyway? Do you really want me digging into your private life? Into your past and history? I am not a victim. I may be a survivor but not in the way you think and not for the reasons you imagine. I am bigger than this. This doesn’t define me.” Dignity, bravery, respect And it may not define most Somali women. I think that’s what confuses many people. Maybe it’s because it happens in childhood and those memories are lost or hidden or maybe because mothers and grandmothers have such good intentions or maybe because it’s so universal within the community? That’s why it’s a completely different experience for a young Somali girl born and brought up somewhere else. The experience is very personal and it varies from person to person. Dignity, respect and bravery are guiding principles for our work on female genital mutilation. In Somaliland, a dynamic young generation connected to the world through the internet, and integrated multi-pronged FGM/C programming, is helping us to influence a generation of Somalis to abandon the cut and break the cycle. It’s still some distance away but we see the end in sight. Words Amal Ahmed, the executive director of our Member Association in Somaliland (SOFHA)

| 19 April 2024
"Dignity, respect and bravery are guiding principles for our work on female genital mutilation (FGM)"
I left Somaliland when I was 9 years old with my mother, brother, uncles, aunts and cousins. It was the civil war and we were lucky enough to reach Canada as refugees. I remember that time as a pleasant, warm, loving time where my cousins and I had a lot of freedom to play, walk to school and daydream. I am from Somaliland so of course I am part of the 97-98% or so of girls who undergo the female genital cut. I think it happened when I was around seven years old. I remember being restrained. I remember strangers being around and I remember peeing standing up and it burning. These memories don’t come up often and they don’t cause me pain. It’s a distant, childhood event. A cousin and a niece my age were there and we went through it together and afterwards our mothers and aunts took care of us. I grew up, went to school, questioned the world and my role in it for a time, got married, had kids and eventually went back to Somaliland. There I met Edna Adan Ismail and asked to volunteer with her. She opened her office, hospital and life to me and I became immersed in the maternal health issues of the women in my home country. The effort to end FGM Most were not as lucky as I had been. Because of FGM/C (female genital mutilation/circumcision), most had experienced recurring infections and difficulties in child birth. Some had formed cysts, some became infertile, and some had obstetric fistula. But few linked these problem to the cutting. At SOFHA (Somaliland Family Health Association) we’ve been working to help women (and men) understand these links and get the help they need. That’s only a part of the work. The effort to end FGM/C in Somaliland goes back almost 40 years. FGM/C programs and projects have been happening for at least the last 25 years. We’re now at the point where it’s recognized as a legitimate, critical, health and social issue. We’re on the cusp of a law against the practice and I have personally witnessed a transformation among the individuals who engage in this work. NGO and government staff tasked with working on FGM/C used to go into communities apologetically, “Sorry but we have to talk to you about this ‘issue’, we know it’s unpleasant but bear with us” to “I have 2 daughters and I have not cut them. This is a terrible practice and we must stop it now”. It fills me with great joy to see young women and men taking this personal stance and doing it confidently and proudly. But it’s not easy for most people to do this. It certainly wasn’t for me. This is personal. This is private. Before I got into the work I might have said, “What business is it of yours anyway? Do you really want me digging into your private life? Into your past and history? I am not a victim. I may be a survivor but not in the way you think and not for the reasons you imagine. I am bigger than this. This doesn’t define me.” Dignity, bravery, respect And it may not define most Somali women. I think that’s what confuses many people. Maybe it’s because it happens in childhood and those memories are lost or hidden or maybe because mothers and grandmothers have such good intentions or maybe because it’s so universal within the community? That’s why it’s a completely different experience for a young Somali girl born and brought up somewhere else. The experience is very personal and it varies from person to person. Dignity, respect and bravery are guiding principles for our work on female genital mutilation. In Somaliland, a dynamic young generation connected to the world through the internet, and integrated multi-pronged FGM/C programming, is helping us to influence a generation of Somalis to abandon the cut and break the cycle. It’s still some distance away but we see the end in sight. Words Amal Ahmed, the executive director of our Member Association in Somaliland (SOFHA)

| 17 November 2017
“The doctors have also been giving me advice on how to look after myself and the baby"
When garment worker Ny thought she might be pregnant with her first child, a home test kit quickly confirmed her suspicions. But the 23-year-old – who is originally from Takeo province but moved to Phnom Penh to take up a job in the garment industry – did not know where to go to seek prenatal care. After a cousin recommended that she visit a nearby Reproductive Health Association of Cambodia clinic, Ny took her relative’s advice – and has gone back eight times to date. “I come here every month to check on the baby,” she says, cradling her belly. “I had never been before I got pregnant.” During her visits to the medical clinic, Ny says, she has had a raft of standard tests and procedures as part of her prenatal care, including two ultrasounds, blood and urine tests, and vaccinations. “The doctors have also been giving me advice on how to look after myself and the baby [such as] to eat nutritious food and not to carry heavy things,” she says. As well as caring for the health of mother and unborn child, RHAC staff have also offered up valuable family planning information. “I did not know about how to plan to have children before I came to the clinic,” Ny says. “The doctors here told me that there are three different methods of [long-term] contraception: medication, an implant and an IUD.” Ny, who sews winter clothing at a factory while her husband also works in a nearby garment factory, says she was very glad to learn about her options. “This child was unplanned, but I don’t feel any regret because I had already been married for two years. But after having the baby I plan to use birth control, though I don’t know what method I will use,” she says. “I know that I don’t want to have another child straight away. It may be two or three years until I have the next one, as I want to wait until my family’s finances improve.”

| 19 April 2024
“The doctors have also been giving me advice on how to look after myself and the baby"
When garment worker Ny thought she might be pregnant with her first child, a home test kit quickly confirmed her suspicions. But the 23-year-old – who is originally from Takeo province but moved to Phnom Penh to take up a job in the garment industry – did not know where to go to seek prenatal care. After a cousin recommended that she visit a nearby Reproductive Health Association of Cambodia clinic, Ny took her relative’s advice – and has gone back eight times to date. “I come here every month to check on the baby,” she says, cradling her belly. “I had never been before I got pregnant.” During her visits to the medical clinic, Ny says, she has had a raft of standard tests and procedures as part of her prenatal care, including two ultrasounds, blood and urine tests, and vaccinations. “The doctors have also been giving me advice on how to look after myself and the baby [such as] to eat nutritious food and not to carry heavy things,” she says. As well as caring for the health of mother and unborn child, RHAC staff have also offered up valuable family planning information. “I did not know about how to plan to have children before I came to the clinic,” Ny says. “The doctors here told me that there are three different methods of [long-term] contraception: medication, an implant and an IUD.” Ny, who sews winter clothing at a factory while her husband also works in a nearby garment factory, says she was very glad to learn about her options. “This child was unplanned, but I don’t feel any regret because I had already been married for two years. But after having the baby I plan to use birth control, though I don’t know what method I will use,” she says. “I know that I don’t want to have another child straight away. It may be two or three years until I have the next one, as I want to wait until my family’s finances improve.”

| 16 November 2017
“When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need"
Female workers, many of them undereducated migrants from rural areas, dominate the garment sector in Cambodia. And Propitious garment factory in Takhmao, a small city that lies just south of the capital Phnom Penh, is no exception. Women make up more than 90 percent of the factory’s workforce. Helping to oversee the 3,700-strong workforce is human resources manager Kouch Davy, who has worked at Propitious since it opened four years ago. Seeing a need to improve the workers’ sexual and reproductive health knowledge, she says she decided to work with the Reproductive Health Association of Cambodia (RHAC) because of its reputation for providing high-quality services. “I raised it in a management meeting, and the board was happy to explore it,” she says. For almost two years, trained staff from RHAC have been visiting the factory twice a month to meet with workers during their lunch break. They answer questions on topics ranging from birth control to STIs and abortion. The organisation has also provided training to the nurses who work in the factory’s on-site medical clinic. Davy says the factory’s female garment workers have changed as a result. “They are more open to asking questions about sexual health and they have also become more informed about the subject,” she says. “When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need, so they tend to exaggerate their problems and ask for sick leave. But when they go to see an RHAC clinic and get proper treatment, there is less sick leave. “Now that they understand about contraception, there are fewer women getting pregnant and taking maternity leave, so that also helps with the workflow. ” Davy says the factory has seen requests for sick leave drop by an average of between 100 to 200 cases a month – and any decrease in absenteeism is a major boon for productivity. “The factory works like a chain: if just one person on the production line takes a day off, it affects the overall productivity,” she says. “And if a worker comes to work sick, they have problems concentrating.” Even Davy says she has gone to RHAC to seek medical care, visiting one of their clinics a few months ago for a breast examination. Meanwhile, the company that owns Propitious has extended its partnership with RHAC to a second factory in Phnom Penh. The firm has even requested that the NGO starts visiting its largest factory, which is situated in a rural province and has 10,000 workers, in the future.

| 19 April 2024
“When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need"
Female workers, many of them undereducated migrants from rural areas, dominate the garment sector in Cambodia. And Propitious garment factory in Takhmao, a small city that lies just south of the capital Phnom Penh, is no exception. Women make up more than 90 percent of the factory’s workforce. Helping to oversee the 3,700-strong workforce is human resources manager Kouch Davy, who has worked at Propitious since it opened four years ago. Seeing a need to improve the workers’ sexual and reproductive health knowledge, she says she decided to work with the Reproductive Health Association of Cambodia (RHAC) because of its reputation for providing high-quality services. “I raised it in a management meeting, and the board was happy to explore it,” she says. For almost two years, trained staff from RHAC have been visiting the factory twice a month to meet with workers during their lunch break. They answer questions on topics ranging from birth control to STIs and abortion. The organisation has also provided training to the nurses who work in the factory’s on-site medical clinic. Davy says the factory’s female garment workers have changed as a result. “They are more open to asking questions about sexual health and they have also become more informed about the subject,” she says. “When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need, so they tend to exaggerate their problems and ask for sick leave. But when they go to see an RHAC clinic and get proper treatment, there is less sick leave. “Now that they understand about contraception, there are fewer women getting pregnant and taking maternity leave, so that also helps with the workflow. ” Davy says the factory has seen requests for sick leave drop by an average of between 100 to 200 cases a month – and any decrease in absenteeism is a major boon for productivity. “The factory works like a chain: if just one person on the production line takes a day off, it affects the overall productivity,” she says. “And if a worker comes to work sick, they have problems concentrating.” Even Davy says she has gone to RHAC to seek medical care, visiting one of their clinics a few months ago for a breast examination. Meanwhile, the company that owns Propitious has extended its partnership with RHAC to a second factory in Phnom Penh. The firm has even requested that the NGO starts visiting its largest factory, which is situated in a rural province and has 10,000 workers, in the future.

| 16 November 2017
"During the pregnancy I was very worried”
Sophorn, a garment worker for the past decade, first visited a Reproductive Health Association of Cambodia (RHAC) clinic when she was pregnant with her first child. She returned for health checks each month until, at five months pregnant, she lost the baby. Her second pregnancy also resulted in a miscarriage, leaving her distraught. Then, she got pregnant a third time, in 2013. “I started to discuss with the doctors how to protect my child,” she says. “They gave me medication to strengthen my cervix, which I took for six months. In the seventh month, I gave birth prematurely.” Doctors told Sophorn that her baby girl was health, but she only weighed in at 1.7 kilograms. The infant was taken to a specialist children’s hospital, where she was cared for an additional two weeks. “During the pregnancy I was very worried,” Sophorn says. “I felt so happy when I finally delivered my child.” Her daughter was born without any complications is now a happy and healthy four years old. In initial stages of her third pregnancy, Sophorn’s friends told her that she would have to undergo surgery on her cervix or have injections to help her carry her baby to term, and doctors at a private clinic confirmed their suggestions. However, she decided to seek a second opinion at RHAC, where doctors instead gave her a prescription to strengthen her cervix. “When I heard I needed to have that surgery I was very scared, so I was relieved when the doctor at RHAC told me to take the medication instead,” she says. “While I was taking the medication I observed my body and any changes to it, so when I felt unwell I would go to the doctors and consult them, so I felt comfortable to continue taking it.” Sophorn also went for appointments at a government-run hospital, but found that their services were also lacking. “I told the doctors about losing my first and second babies, but they only weighed me and measured my stomach. There weren’t any more examinations or very much care,” she says. “When I went to RHAC they did so many examinations and had so many services, so I think it’s really better to go to RHAC for these kinds of services.” She estimates that during her third pregnancy, she had ten appointments at RHAC clinics at a cost of 40,000 to 60,000 riel (£7.40 to £11.15) each time. Compared to just 2,000 riel for an obstetrics appointment at the public hospital, the difference in cost is significant. “It’s expensive for me because my salary is little.” Despite the relatively high prices, Sophorn already knows where she will go for medical care in the future. “I want to have one more child, and I have already planned that when I decide to do it I will go to RHAC to get my cervix checked first,” she says. Until that day comes, Sophorn is taking the oral contraceptive after receiving advice about birth control from RHAC’s clinicians, with a midwife from the NGO making regular visits to the factory.

| 19 April 2024
"During the pregnancy I was very worried”
Sophorn, a garment worker for the past decade, first visited a Reproductive Health Association of Cambodia (RHAC) clinic when she was pregnant with her first child. She returned for health checks each month until, at five months pregnant, she lost the baby. Her second pregnancy also resulted in a miscarriage, leaving her distraught. Then, she got pregnant a third time, in 2013. “I started to discuss with the doctors how to protect my child,” she says. “They gave me medication to strengthen my cervix, which I took for six months. In the seventh month, I gave birth prematurely.” Doctors told Sophorn that her baby girl was health, but she only weighed in at 1.7 kilograms. The infant was taken to a specialist children’s hospital, where she was cared for an additional two weeks. “During the pregnancy I was very worried,” Sophorn says. “I felt so happy when I finally delivered my child.” Her daughter was born without any complications is now a happy and healthy four years old. In initial stages of her third pregnancy, Sophorn’s friends told her that she would have to undergo surgery on her cervix or have injections to help her carry her baby to term, and doctors at a private clinic confirmed their suggestions. However, she decided to seek a second opinion at RHAC, where doctors instead gave her a prescription to strengthen her cervix. “When I heard I needed to have that surgery I was very scared, so I was relieved when the doctor at RHAC told me to take the medication instead,” she says. “While I was taking the medication I observed my body and any changes to it, so when I felt unwell I would go to the doctors and consult them, so I felt comfortable to continue taking it.” Sophorn also went for appointments at a government-run hospital, but found that their services were also lacking. “I told the doctors about losing my first and second babies, but they only weighed me and measured my stomach. There weren’t any more examinations or very much care,” she says. “When I went to RHAC they did so many examinations and had so many services, so I think it’s really better to go to RHAC for these kinds of services.” She estimates that during her third pregnancy, she had ten appointments at RHAC clinics at a cost of 40,000 to 60,000 riel (£7.40 to £11.15) each time. Compared to just 2,000 riel for an obstetrics appointment at the public hospital, the difference in cost is significant. “It’s expensive for me because my salary is little.” Despite the relatively high prices, Sophorn already knows where she will go for medical care in the future. “I want to have one more child, and I have already planned that when I decide to do it I will go to RHAC to get my cervix checked first,” she says. Until that day comes, Sophorn is taking the oral contraceptive after receiving advice about birth control from RHAC’s clinicians, with a midwife from the NGO making regular visits to the factory.

| 18 December 2018
"Many of the women we work with have no health insurance"
Hatixhe Gorenca is a nurse at the Albanian Centre of Population and Development (ACPD) clinic in Tirana. She joined the center in 2013 with 39 years of experience working in gynaecology. During her time as a nurse, she has seen vast improvements in access and services for cervical cancer screenings. However, she says that there is a considerable number of women in rural areas that face difficulties in accessing healthcare, and some that cannot access it at all. Rural women & access “The ACPD clinic is crucial for these [rural] women, because the healthcare we offer through gynaecological visits, includes counselling, pap smears, colposcopies and recently VIA tests and cryotherapy. Services that are totally missing in their areas. What they appreciate most is the mobile clinic in the outskirts of Tirana, because they have an opportunity to meet with doctors and to get information about their health status. We do approximately 17-18 visits per day and the number is always increasing”, Hatixhe says. The clinic has developed a reputation for offering youth-friendly healthcare and information. The confidential and open approach of the clinic is providing access for girls to comprehensive sexual education at an early age, without fear of discrimination or embarrassment. When the clinic first introduced VIA testing in 2017, as an alternative way for the screening of cervical cancer, it was welcomed by the women. “The reason is that compared to pap smears, VIA gives an immediate response on the health of the cervical cells,” Hatixhe explains. “The other reason is economical. Many of the women we work with have no health insurance, as such they cannot benefit from the free tests at maternity hospitals. Furthermore, some of them are vulnerable women and they feel safe when they can get free information and healthcare at our clinic.” What is VIA & Cryotherapy? Show more + Visual inspection of the cervix with acetic acid (VIA) is a process of screening and examining the cervix. Pre-cancerous lesions on the cervix will turn white when the acid is applied. This simple procedure can be done in a clinic setting without the use of a laboratory and allows for immediate treatment of any pre-cancerous lesions with cryotherapy. Cryotherapy is a gynaecological treatment that freezes and destroys abnormal, pre-cancerous cervical cells. Cryotherapy is not a treatment for cervical cancer. VIA has the potential to revolutionize cervical cancer prevention efforts, particularly in low resource settings, because it eliminates the need for laboratories, transportation of specimens and provides immediate test results. VIA needs less equipment and fewer specialists than traditional cervical cancer screening methods like Pap smears. Results from VIA are available immediately so women can be screened and treated in one single visit. ACDP outreach activities enable the staff to give the information where the women are: in the streets, in their workplace, in their homes. Hatixhe has witnessed a growing interest in women regarding their reproductive health in recent years. The number of women that walk through the clinic doors is proof of that. During the 2016-2017 over 3,000 women received healthcare services from the clinic. Encouraging other women “I myself am learning a lot in the clinic”, Hatixhe says. “VIA test was a new technique even for me, but it is so simple, I can now train the staff at the health centers. I can tell you that they are very enthusiastic and responsive because VIA is very easy to apply. Since many health centers have no gynaecological bed for their visits or low capacities to apply PAP tests which require specialized personnel, VIA is much more suitable for their conditions, because it can be done by the nurses or midwifes themselves.” Hatixhe is impressed by the reaction of women taking VIA tests. “As a nurse with long experience in the health sector, I have received many thanks from patients, but the hugs we get from these women are heartfelt. After 2-3 years of coming and going to different institutions, finally, they have found a method which can detect pre-cancer cells, get treatment for it and now they are totally healthy.” Hatixhe says that many women have been encouraged to book a VIA test through hearing about it from a friend or relative who had a positive experience at the clinic. “After the first visit, the women return with other women who are interested to do the tests. This is wonderful.”

| 19 April 2024
"Many of the women we work with have no health insurance"
Hatixhe Gorenca is a nurse at the Albanian Centre of Population and Development (ACPD) clinic in Tirana. She joined the center in 2013 with 39 years of experience working in gynaecology. During her time as a nurse, she has seen vast improvements in access and services for cervical cancer screenings. However, she says that there is a considerable number of women in rural areas that face difficulties in accessing healthcare, and some that cannot access it at all. Rural women & access “The ACPD clinic is crucial for these [rural] women, because the healthcare we offer through gynaecological visits, includes counselling, pap smears, colposcopies and recently VIA tests and cryotherapy. Services that are totally missing in their areas. What they appreciate most is the mobile clinic in the outskirts of Tirana, because they have an opportunity to meet with doctors and to get information about their health status. We do approximately 17-18 visits per day and the number is always increasing”, Hatixhe says. The clinic has developed a reputation for offering youth-friendly healthcare and information. The confidential and open approach of the clinic is providing access for girls to comprehensive sexual education at an early age, without fear of discrimination or embarrassment. When the clinic first introduced VIA testing in 2017, as an alternative way for the screening of cervical cancer, it was welcomed by the women. “The reason is that compared to pap smears, VIA gives an immediate response on the health of the cervical cells,” Hatixhe explains. “The other reason is economical. Many of the women we work with have no health insurance, as such they cannot benefit from the free tests at maternity hospitals. Furthermore, some of them are vulnerable women and they feel safe when they can get free information and healthcare at our clinic.” What is VIA & Cryotherapy? Show more + Visual inspection of the cervix with acetic acid (VIA) is a process of screening and examining the cervix. Pre-cancerous lesions on the cervix will turn white when the acid is applied. This simple procedure can be done in a clinic setting without the use of a laboratory and allows for immediate treatment of any pre-cancerous lesions with cryotherapy. Cryotherapy is a gynaecological treatment that freezes and destroys abnormal, pre-cancerous cervical cells. Cryotherapy is not a treatment for cervical cancer. VIA has the potential to revolutionize cervical cancer prevention efforts, particularly in low resource settings, because it eliminates the need for laboratories, transportation of specimens and provides immediate test results. VIA needs less equipment and fewer specialists than traditional cervical cancer screening methods like Pap smears. Results from VIA are available immediately so women can be screened and treated in one single visit. ACDP outreach activities enable the staff to give the information where the women are: in the streets, in their workplace, in their homes. Hatixhe has witnessed a growing interest in women regarding their reproductive health in recent years. The number of women that walk through the clinic doors is proof of that. During the 2016-2017 over 3,000 women received healthcare services from the clinic. Encouraging other women “I myself am learning a lot in the clinic”, Hatixhe says. “VIA test was a new technique even for me, but it is so simple, I can now train the staff at the health centers. I can tell you that they are very enthusiastic and responsive because VIA is very easy to apply. Since many health centers have no gynaecological bed for their visits or low capacities to apply PAP tests which require specialized personnel, VIA is much more suitable for their conditions, because it can be done by the nurses or midwifes themselves.” Hatixhe is impressed by the reaction of women taking VIA tests. “As a nurse with long experience in the health sector, I have received many thanks from patients, but the hugs we get from these women are heartfelt. After 2-3 years of coming and going to different institutions, finally, they have found a method which can detect pre-cancer cells, get treatment for it and now they are totally healthy.” Hatixhe says that many women have been encouraged to book a VIA test through hearing about it from a friend or relative who had a positive experience at the clinic. “After the first visit, the women return with other women who are interested to do the tests. This is wonderful.”
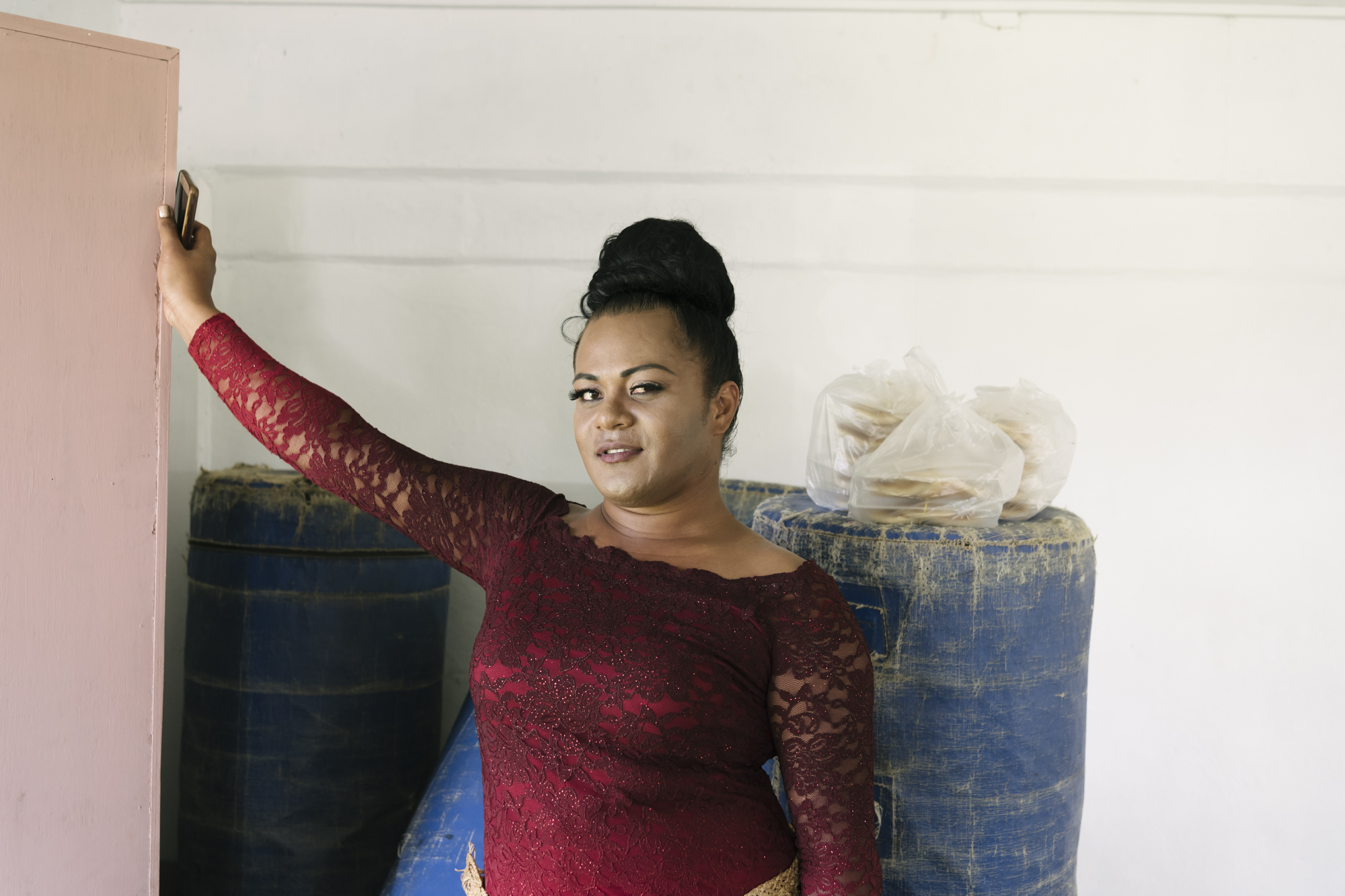
| 29 March 2018
"I have a feeling the future will be better"
Leiti is a Tongan word to describe transgender women, it comes from the English word “lady”. In Tonga the transgender community is organized by the Tonga Leiti Association (TLA), and with the support of Tonga Family Health Association (TFHA). Together they are educating people to help stop the discrimination and stigma surrounding the Leiti community. Leilani, who identifies as a leiti, has been working with the Tonga Leiti Association, supported by Tonga Health Family Association to battle the stigma surrounding the leiti and LGBTI+ community in Tonga. She says "I started to dress like a leiti at a very young age. Being a leiti in a Tongan family is very difficult because being a leiti or having a son who’s a leiti are considered shameful, so for the family (it) is very difficult to accept us. Many leitis run away from their families." Frequently facing abuse Access to health care and sexual and reproductive health service is another difficulty the leiti community face: going to public clinics, they often face abuse and are more likely to be ignored or dismissed by staff. When they are turned away from other clinics, Leilani knows she can always rely on Tonga Health Family Association for help. 'I think Tonga Family Health has done a lot up to now. They always come and do our annual HIV testing and they supply us (with) some condom because we do the condom distribution here in Tonga and if we have a case in our members or anybody come to our office we refer them to Tonga Family Health. They really, really help us a lot. They (are the) only one that can understand us." Tonga Family Health Association and Tonga Leiti Association partnership allows for both organisations to attend training workshops run by one another. A valuable opportunity not only for clinic staff but for volunteers like Leilani. "When the Tonga Family Health run the training they always ask some members from TLA to come and train with them and we do the same with them. When I give a presentation at the TFHA's clinic, I share with people what we do; I ask them for to change their mindset and how they look about us." Overcoming stigma and discrimination With her training, Leilani visits schools to help educate, inform and overcome the stigma and discrimination surrounding the leiti community. Many young leiti's drop out of school at an early age due to verbal, physical and in some cases sexual abuse. Slowly, Leilani is seeing a positive change in the schools she visits. “We go to school because there a lot of discrimination of the leiti's in high school and primary school too. I have been going from school to school for two years. My plan to visit all the schools in Tonga. We mostly go to all-boys schools is because discrimination in school is mostly done by boys. I was very happy last year when I went to a boys school and so how they really appreciate the work and how well they treated the Leiti's in the school." In February, Tonga was hit by tropical cyclone Gita, the worst cyclone to hit the island in over 60 years. Leilani worries that not enough is being done to ensure the needs of the Leiti and LGBTI+ community is being met during and post humanitarian disasters. "We are one of the vulnerable groups, after the cyclone Gita we should be one of the first priority for the government, or the hospital or any donations. Cause our life is very unique and we are easy to harm." Despite the hardships surrounding the leiti community, Leilani is hopeful for the future, "I can see a lot of families that now accept leiti's in their house and they treat them well. I have a feeling the future will be better. Please stop discriminating against us, but love us. We are here to stay, we are not here to chase away." Watch the Humanitarian teams response to Cyclone Gita
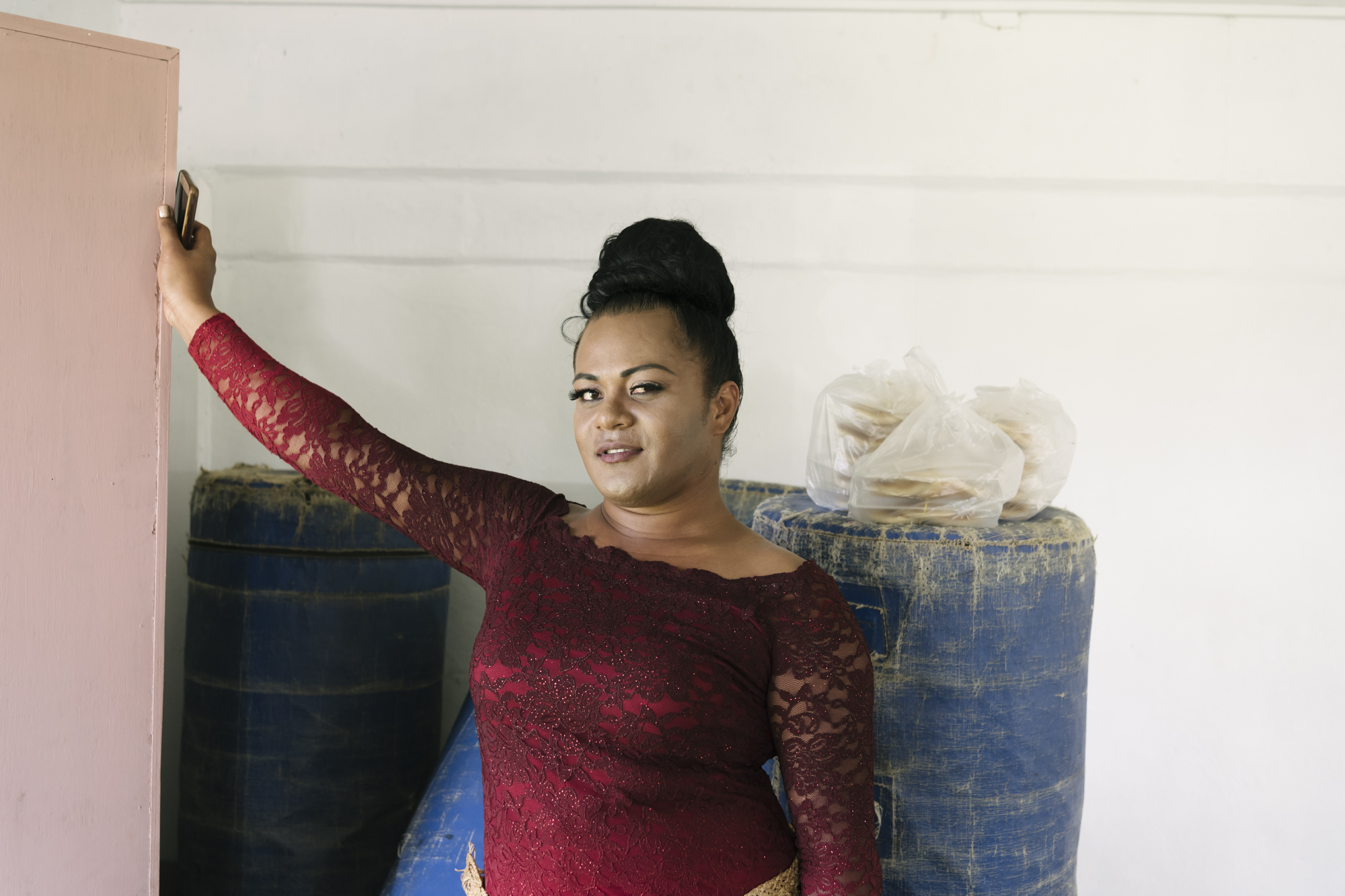
| 19 April 2024
"I have a feeling the future will be better"
Leiti is a Tongan word to describe transgender women, it comes from the English word “lady”. In Tonga the transgender community is organized by the Tonga Leiti Association (TLA), and with the support of Tonga Family Health Association (TFHA). Together they are educating people to help stop the discrimination and stigma surrounding the Leiti community. Leilani, who identifies as a leiti, has been working with the Tonga Leiti Association, supported by Tonga Health Family Association to battle the stigma surrounding the leiti and LGBTI+ community in Tonga. She says "I started to dress like a leiti at a very young age. Being a leiti in a Tongan family is very difficult because being a leiti or having a son who’s a leiti are considered shameful, so for the family (it) is very difficult to accept us. Many leitis run away from their families." Frequently facing abuse Access to health care and sexual and reproductive health service is another difficulty the leiti community face: going to public clinics, they often face abuse and are more likely to be ignored or dismissed by staff. When they are turned away from other clinics, Leilani knows she can always rely on Tonga Health Family Association for help. 'I think Tonga Family Health has done a lot up to now. They always come and do our annual HIV testing and they supply us (with) some condom because we do the condom distribution here in Tonga and if we have a case in our members or anybody come to our office we refer them to Tonga Family Health. They really, really help us a lot. They (are the) only one that can understand us." Tonga Family Health Association and Tonga Leiti Association partnership allows for both organisations to attend training workshops run by one another. A valuable opportunity not only for clinic staff but for volunteers like Leilani. "When the Tonga Family Health run the training they always ask some members from TLA to come and train with them and we do the same with them. When I give a presentation at the TFHA's clinic, I share with people what we do; I ask them for to change their mindset and how they look about us." Overcoming stigma and discrimination With her training, Leilani visits schools to help educate, inform and overcome the stigma and discrimination surrounding the leiti community. Many young leiti's drop out of school at an early age due to verbal, physical and in some cases sexual abuse. Slowly, Leilani is seeing a positive change in the schools she visits. “We go to school because there a lot of discrimination of the leiti's in high school and primary school too. I have been going from school to school for two years. My plan to visit all the schools in Tonga. We mostly go to all-boys schools is because discrimination in school is mostly done by boys. I was very happy last year when I went to a boys school and so how they really appreciate the work and how well they treated the Leiti's in the school." In February, Tonga was hit by tropical cyclone Gita, the worst cyclone to hit the island in over 60 years. Leilani worries that not enough is being done to ensure the needs of the Leiti and LGBTI+ community is being met during and post humanitarian disasters. "We are one of the vulnerable groups, after the cyclone Gita we should be one of the first priority for the government, or the hospital or any donations. Cause our life is very unique and we are easy to harm." Despite the hardships surrounding the leiti community, Leilani is hopeful for the future, "I can see a lot of families that now accept leiti's in their house and they treat them well. I have a feeling the future will be better. Please stop discriminating against us, but love us. We are here to stay, we are not here to chase away." Watch the Humanitarian teams response to Cyclone Gita

| 05 February 2018
"Dignity, respect and bravery are guiding principles for our work on female genital mutilation (FGM)"
I left Somaliland when I was 9 years old with my mother, brother, uncles, aunts and cousins. It was the civil war and we were lucky enough to reach Canada as refugees. I remember that time as a pleasant, warm, loving time where my cousins and I had a lot of freedom to play, walk to school and daydream. I am from Somaliland so of course I am part of the 97-98% or so of girls who undergo the female genital cut. I think it happened when I was around seven years old. I remember being restrained. I remember strangers being around and I remember peeing standing up and it burning. These memories don’t come up often and they don’t cause me pain. It’s a distant, childhood event. A cousin and a niece my age were there and we went through it together and afterwards our mothers and aunts took care of us. I grew up, went to school, questioned the world and my role in it for a time, got married, had kids and eventually went back to Somaliland. There I met Edna Adan Ismail and asked to volunteer with her. She opened her office, hospital and life to me and I became immersed in the maternal health issues of the women in my home country. The effort to end FGM Most were not as lucky as I had been. Because of FGM/C (female genital mutilation/circumcision), most had experienced recurring infections and difficulties in child birth. Some had formed cysts, some became infertile, and some had obstetric fistula. But few linked these problem to the cutting. At SOFHA (Somaliland Family Health Association) we’ve been working to help women (and men) understand these links and get the help they need. That’s only a part of the work. The effort to end FGM/C in Somaliland goes back almost 40 years. FGM/C programs and projects have been happening for at least the last 25 years. We’re now at the point where it’s recognized as a legitimate, critical, health and social issue. We’re on the cusp of a law against the practice and I have personally witnessed a transformation among the individuals who engage in this work. NGO and government staff tasked with working on FGM/C used to go into communities apologetically, “Sorry but we have to talk to you about this ‘issue’, we know it’s unpleasant but bear with us” to “I have 2 daughters and I have not cut them. This is a terrible practice and we must stop it now”. It fills me with great joy to see young women and men taking this personal stance and doing it confidently and proudly. But it’s not easy for most people to do this. It certainly wasn’t for me. This is personal. This is private. Before I got into the work I might have said, “What business is it of yours anyway? Do you really want me digging into your private life? Into your past and history? I am not a victim. I may be a survivor but not in the way you think and not for the reasons you imagine. I am bigger than this. This doesn’t define me.” Dignity, bravery, respect And it may not define most Somali women. I think that’s what confuses many people. Maybe it’s because it happens in childhood and those memories are lost or hidden or maybe because mothers and grandmothers have such good intentions or maybe because it’s so universal within the community? That’s why it’s a completely different experience for a young Somali girl born and brought up somewhere else. The experience is very personal and it varies from person to person. Dignity, respect and bravery are guiding principles for our work on female genital mutilation. In Somaliland, a dynamic young generation connected to the world through the internet, and integrated multi-pronged FGM/C programming, is helping us to influence a generation of Somalis to abandon the cut and break the cycle. It’s still some distance away but we see the end in sight. Words Amal Ahmed, the executive director of our Member Association in Somaliland (SOFHA)

| 19 April 2024
"Dignity, respect and bravery are guiding principles for our work on female genital mutilation (FGM)"
I left Somaliland when I was 9 years old with my mother, brother, uncles, aunts and cousins. It was the civil war and we were lucky enough to reach Canada as refugees. I remember that time as a pleasant, warm, loving time where my cousins and I had a lot of freedom to play, walk to school and daydream. I am from Somaliland so of course I am part of the 97-98% or so of girls who undergo the female genital cut. I think it happened when I was around seven years old. I remember being restrained. I remember strangers being around and I remember peeing standing up and it burning. These memories don’t come up often and they don’t cause me pain. It’s a distant, childhood event. A cousin and a niece my age were there and we went through it together and afterwards our mothers and aunts took care of us. I grew up, went to school, questioned the world and my role in it for a time, got married, had kids and eventually went back to Somaliland. There I met Edna Adan Ismail and asked to volunteer with her. She opened her office, hospital and life to me and I became immersed in the maternal health issues of the women in my home country. The effort to end FGM Most were not as lucky as I had been. Because of FGM/C (female genital mutilation/circumcision), most had experienced recurring infections and difficulties in child birth. Some had formed cysts, some became infertile, and some had obstetric fistula. But few linked these problem to the cutting. At SOFHA (Somaliland Family Health Association) we’ve been working to help women (and men) understand these links and get the help they need. That’s only a part of the work. The effort to end FGM/C in Somaliland goes back almost 40 years. FGM/C programs and projects have been happening for at least the last 25 years. We’re now at the point where it’s recognized as a legitimate, critical, health and social issue. We’re on the cusp of a law against the practice and I have personally witnessed a transformation among the individuals who engage in this work. NGO and government staff tasked with working on FGM/C used to go into communities apologetically, “Sorry but we have to talk to you about this ‘issue’, we know it’s unpleasant but bear with us” to “I have 2 daughters and I have not cut them. This is a terrible practice and we must stop it now”. It fills me with great joy to see young women and men taking this personal stance and doing it confidently and proudly. But it’s not easy for most people to do this. It certainly wasn’t for me. This is personal. This is private. Before I got into the work I might have said, “What business is it of yours anyway? Do you really want me digging into your private life? Into your past and history? I am not a victim. I may be a survivor but not in the way you think and not for the reasons you imagine. I am bigger than this. This doesn’t define me.” Dignity, bravery, respect And it may not define most Somali women. I think that’s what confuses many people. Maybe it’s because it happens in childhood and those memories are lost or hidden or maybe because mothers and grandmothers have such good intentions or maybe because it’s so universal within the community? That’s why it’s a completely different experience for a young Somali girl born and brought up somewhere else. The experience is very personal and it varies from person to person. Dignity, respect and bravery are guiding principles for our work on female genital mutilation. In Somaliland, a dynamic young generation connected to the world through the internet, and integrated multi-pronged FGM/C programming, is helping us to influence a generation of Somalis to abandon the cut and break the cycle. It’s still some distance away but we see the end in sight. Words Amal Ahmed, the executive director of our Member Association in Somaliland (SOFHA)

| 17 November 2017
“The doctors have also been giving me advice on how to look after myself and the baby"
When garment worker Ny thought she might be pregnant with her first child, a home test kit quickly confirmed her suspicions. But the 23-year-old – who is originally from Takeo province but moved to Phnom Penh to take up a job in the garment industry – did not know where to go to seek prenatal care. After a cousin recommended that she visit a nearby Reproductive Health Association of Cambodia clinic, Ny took her relative’s advice – and has gone back eight times to date. “I come here every month to check on the baby,” she says, cradling her belly. “I had never been before I got pregnant.” During her visits to the medical clinic, Ny says, she has had a raft of standard tests and procedures as part of her prenatal care, including two ultrasounds, blood and urine tests, and vaccinations. “The doctors have also been giving me advice on how to look after myself and the baby [such as] to eat nutritious food and not to carry heavy things,” she says. As well as caring for the health of mother and unborn child, RHAC staff have also offered up valuable family planning information. “I did not know about how to plan to have children before I came to the clinic,” Ny says. “The doctors here told me that there are three different methods of [long-term] contraception: medication, an implant and an IUD.” Ny, who sews winter clothing at a factory while her husband also works in a nearby garment factory, says she was very glad to learn about her options. “This child was unplanned, but I don’t feel any regret because I had already been married for two years. But after having the baby I plan to use birth control, though I don’t know what method I will use,” she says. “I know that I don’t want to have another child straight away. It may be two or three years until I have the next one, as I want to wait until my family’s finances improve.”

| 19 April 2024
“The doctors have also been giving me advice on how to look after myself and the baby"
When garment worker Ny thought she might be pregnant with her first child, a home test kit quickly confirmed her suspicions. But the 23-year-old – who is originally from Takeo province but moved to Phnom Penh to take up a job in the garment industry – did not know where to go to seek prenatal care. After a cousin recommended that she visit a nearby Reproductive Health Association of Cambodia clinic, Ny took her relative’s advice – and has gone back eight times to date. “I come here every month to check on the baby,” she says, cradling her belly. “I had never been before I got pregnant.” During her visits to the medical clinic, Ny says, she has had a raft of standard tests and procedures as part of her prenatal care, including two ultrasounds, blood and urine tests, and vaccinations. “The doctors have also been giving me advice on how to look after myself and the baby [such as] to eat nutritious food and not to carry heavy things,” she says. As well as caring for the health of mother and unborn child, RHAC staff have also offered up valuable family planning information. “I did not know about how to plan to have children before I came to the clinic,” Ny says. “The doctors here told me that there are three different methods of [long-term] contraception: medication, an implant and an IUD.” Ny, who sews winter clothing at a factory while her husband also works in a nearby garment factory, says she was very glad to learn about her options. “This child was unplanned, but I don’t feel any regret because I had already been married for two years. But after having the baby I plan to use birth control, though I don’t know what method I will use,” she says. “I know that I don’t want to have another child straight away. It may be two or three years until I have the next one, as I want to wait until my family’s finances improve.”

| 16 November 2017
“When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need"
Female workers, many of them undereducated migrants from rural areas, dominate the garment sector in Cambodia. And Propitious garment factory in Takhmao, a small city that lies just south of the capital Phnom Penh, is no exception. Women make up more than 90 percent of the factory’s workforce. Helping to oversee the 3,700-strong workforce is human resources manager Kouch Davy, who has worked at Propitious since it opened four years ago. Seeing a need to improve the workers’ sexual and reproductive health knowledge, she says she decided to work with the Reproductive Health Association of Cambodia (RHAC) because of its reputation for providing high-quality services. “I raised it in a management meeting, and the board was happy to explore it,” she says. For almost two years, trained staff from RHAC have been visiting the factory twice a month to meet with workers during their lunch break. They answer questions on topics ranging from birth control to STIs and abortion. The organisation has also provided training to the nurses who work in the factory’s on-site medical clinic. Davy says the factory’s female garment workers have changed as a result. “They are more open to asking questions about sexual health and they have also become more informed about the subject,” she says. “When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need, so they tend to exaggerate their problems and ask for sick leave. But when they go to see an RHAC clinic and get proper treatment, there is less sick leave. “Now that they understand about contraception, there are fewer women getting pregnant and taking maternity leave, so that also helps with the workflow. ” Davy says the factory has seen requests for sick leave drop by an average of between 100 to 200 cases a month – and any decrease in absenteeism is a major boon for productivity. “The factory works like a chain: if just one person on the production line takes a day off, it affects the overall productivity,” she says. “And if a worker comes to work sick, they have problems concentrating.” Even Davy says she has gone to RHAC to seek medical care, visiting one of their clinics a few months ago for a breast examination. Meanwhile, the company that owns Propitious has extended its partnership with RHAC to a second factory in Phnom Penh. The firm has even requested that the NGO starts visiting its largest factory, which is situated in a rural province and has 10,000 workers, in the future.

| 19 April 2024
“When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need"
Female workers, many of them undereducated migrants from rural areas, dominate the garment sector in Cambodia. And Propitious garment factory in Takhmao, a small city that lies just south of the capital Phnom Penh, is no exception. Women make up more than 90 percent of the factory’s workforce. Helping to oversee the 3,700-strong workforce is human resources manager Kouch Davy, who has worked at Propitious since it opened four years ago. Seeing a need to improve the workers’ sexual and reproductive health knowledge, she says she decided to work with the Reproductive Health Association of Cambodia (RHAC) because of its reputation for providing high-quality services. “I raised it in a management meeting, and the board was happy to explore it,” she says. For almost two years, trained staff from RHAC have been visiting the factory twice a month to meet with workers during their lunch break. They answer questions on topics ranging from birth control to STIs and abortion. The organisation has also provided training to the nurses who work in the factory’s on-site medical clinic. Davy says the factory’s female garment workers have changed as a result. “They are more open to asking questions about sexual health and they have also become more informed about the subject,” she says. “When they don’t dare to ask questions about sensitive health topics, they don’t have the information they need, so they tend to exaggerate their problems and ask for sick leave. But when they go to see an RHAC clinic and get proper treatment, there is less sick leave. “Now that they understand about contraception, there are fewer women getting pregnant and taking maternity leave, so that also helps with the workflow. ” Davy says the factory has seen requests for sick leave drop by an average of between 100 to 200 cases a month – and any decrease in absenteeism is a major boon for productivity. “The factory works like a chain: if just one person on the production line takes a day off, it affects the overall productivity,” she says. “And if a worker comes to work sick, they have problems concentrating.” Even Davy says she has gone to RHAC to seek medical care, visiting one of their clinics a few months ago for a breast examination. Meanwhile, the company that owns Propitious has extended its partnership with RHAC to a second factory in Phnom Penh. The firm has even requested that the NGO starts visiting its largest factory, which is situated in a rural province and has 10,000 workers, in the future.

| 16 November 2017
"During the pregnancy I was very worried”
Sophorn, a garment worker for the past decade, first visited a Reproductive Health Association of Cambodia (RHAC) clinic when she was pregnant with her first child. She returned for health checks each month until, at five months pregnant, she lost the baby. Her second pregnancy also resulted in a miscarriage, leaving her distraught. Then, she got pregnant a third time, in 2013. “I started to discuss with the doctors how to protect my child,” she says. “They gave me medication to strengthen my cervix, which I took for six months. In the seventh month, I gave birth prematurely.” Doctors told Sophorn that her baby girl was health, but she only weighed in at 1.7 kilograms. The infant was taken to a specialist children’s hospital, where she was cared for an additional two weeks. “During the pregnancy I was very worried,” Sophorn says. “I felt so happy when I finally delivered my child.” Her daughter was born without any complications is now a happy and healthy four years old. In initial stages of her third pregnancy, Sophorn’s friends told her that she would have to undergo surgery on her cervix or have injections to help her carry her baby to term, and doctors at a private clinic confirmed their suggestions. However, she decided to seek a second opinion at RHAC, where doctors instead gave her a prescription to strengthen her cervix. “When I heard I needed to have that surgery I was very scared, so I was relieved when the doctor at RHAC told me to take the medication instead,” she says. “While I was taking the medication I observed my body and any changes to it, so when I felt unwell I would go to the doctors and consult them, so I felt comfortable to continue taking it.” Sophorn also went for appointments at a government-run hospital, but found that their services were also lacking. “I told the doctors about losing my first and second babies, but they only weighed me and measured my stomach. There weren’t any more examinations or very much care,” she says. “When I went to RHAC they did so many examinations and had so many services, so I think it’s really better to go to RHAC for these kinds of services.” She estimates that during her third pregnancy, she had ten appointments at RHAC clinics at a cost of 40,000 to 60,000 riel (£7.40 to £11.15) each time. Compared to just 2,000 riel for an obstetrics appointment at the public hospital, the difference in cost is significant. “It’s expensive for me because my salary is little.” Despite the relatively high prices, Sophorn already knows where she will go for medical care in the future. “I want to have one more child, and I have already planned that when I decide to do it I will go to RHAC to get my cervix checked first,” she says. Until that day comes, Sophorn is taking the oral contraceptive after receiving advice about birth control from RHAC’s clinicians, with a midwife from the NGO making regular visits to the factory.

| 19 April 2024
"During the pregnancy I was very worried”
Sophorn, a garment worker for the past decade, first visited a Reproductive Health Association of Cambodia (RHAC) clinic when she was pregnant with her first child. She returned for health checks each month until, at five months pregnant, she lost the baby. Her second pregnancy also resulted in a miscarriage, leaving her distraught. Then, she got pregnant a third time, in 2013. “I started to discuss with the doctors how to protect my child,” she says. “They gave me medication to strengthen my cervix, which I took for six months. In the seventh month, I gave birth prematurely.” Doctors told Sophorn that her baby girl was health, but she only weighed in at 1.7 kilograms. The infant was taken to a specialist children’s hospital, where she was cared for an additional two weeks. “During the pregnancy I was very worried,” Sophorn says. “I felt so happy when I finally delivered my child.” Her daughter was born without any complications is now a happy and healthy four years old. In initial stages of her third pregnancy, Sophorn’s friends told her that she would have to undergo surgery on her cervix or have injections to help her carry her baby to term, and doctors at a private clinic confirmed their suggestions. However, she decided to seek a second opinion at RHAC, where doctors instead gave her a prescription to strengthen her cervix. “When I heard I needed to have that surgery I was very scared, so I was relieved when the doctor at RHAC told me to take the medication instead,” she says. “While I was taking the medication I observed my body and any changes to it, so when I felt unwell I would go to the doctors and consult them, so I felt comfortable to continue taking it.” Sophorn also went for appointments at a government-run hospital, but found that their services were also lacking. “I told the doctors about losing my first and second babies, but they only weighed me and measured my stomach. There weren’t any more examinations or very much care,” she says. “When I went to RHAC they did so many examinations and had so many services, so I think it’s really better to go to RHAC for these kinds of services.” She estimates that during her third pregnancy, she had ten appointments at RHAC clinics at a cost of 40,000 to 60,000 riel (£7.40 to £11.15) each time. Compared to just 2,000 riel for an obstetrics appointment at the public hospital, the difference in cost is significant. “It’s expensive for me because my salary is little.” Despite the relatively high prices, Sophorn already knows where she will go for medical care in the future. “I want to have one more child, and I have already planned that when I decide to do it I will go to RHAC to get my cervix checked first,” she says. Until that day comes, Sophorn is taking the oral contraceptive after receiving advice about birth control from RHAC’s clinicians, with a midwife from the NGO making regular visits to the factory.








