The past 15 years have been turbulent for this small, landlocked country. Poverty is widespread and the earthquake of 2015 had a devastating effect. Almost 9,000 people were killed and over 22,000 injured, while the effect on houses and buildings was catastrophic: around 800,000 homes were destroyed or damaged, and 3 million people were displaced.
The earthquake hit Nepal’s health sector hard. Clinics were destroyed up and down the country, and for the millions displaced from home and forced into tents, accessing health services – including family planning – became difficult, sometimes impossible.

Contraception and family planning: the issues
Even before the earthquake, family planning in Nepal was fraught with problems. Around 14 million Nepalis live in mountainous or hilly regions, often in small, remote villages many miles from the nearest town, where health facilities are often scarce, understaffed and poorly supplied with drugs. Where roads exist, they are often potholed, sometimes impassable, making road travel arduous. For the millions of Nepalis living beneath or near the poverty line, travelling on foot is the only option, and, even when they can afford to rent a space in a car, vehicles are scarce.
“When I was about to give birth, we called for an ambulance or a vehicle to help but even after five hours of calling, no vehicle arrived,” recalls 32-year-old Muna Shrestha. “The birth was difficult. For five hours I suffered from delivery problems.”
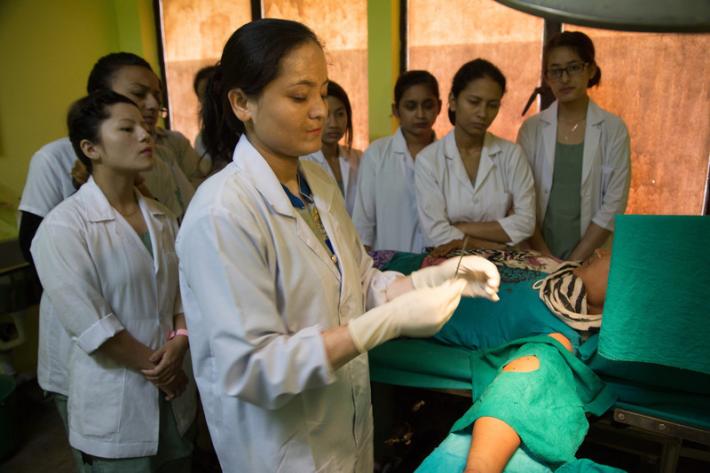
Every year, tens of thousands of Nepalis give birth without any medical help at all: just 36% of births are attended by a doctor, nurse or midwife. Maternal mortality is one of the leading causes of death among women.
Myths, misconceptions and cultural resistance to contraception
A lack of knowledge about family planning and contraception compounds the issue – a problem that becomes even greater among Nepal’s many rural communities and certain ethnic groups.
In thousands of households, hostility towards family planning has its roots in deep-rooted customs and beliefs. In Nepal’s largely patriarchal culture, it remains the norm for couples to have four or more children: preference for sons means women are forced to go on having children until boys are born. Contraception remains an alien, uncomfortable idea for millions of Nepalis and is tightly controlled by men: women often need consent from their husbands to use contraception.

Misconceptions are also rife. “I’ve heard the coil can cause cancer,” says Muna Shrestha, a farmer from Kavre district. “There are so many side effects to these devices.”
In many households, contraception is deemed to fly in the face of ancient cultural traditions. “It’s thought that men who have had vasectomies won’t be able to perform the rituals after their parent’s death,” explains Binu. “Parents think that
God won’t accept that, so they don’t allow men to have vasectomies.”
Pasang Tamang, an FPAN volunteer in Gatlang, tells of one man who threatened to kill his wife, the doctor and any health worker who provided family planning services to his wife.
Spreading knowledge to remote regions
Meeting the family planning needs of Nepal’s 28 million people, particularly those living in remote mountain villages, takes careful planning, complex logistics, skilled staff and money. Since 1959, the Family Planning Association of Nepal (FPAN), has been providing better access to family planning and maternal health, ensuring its services penetrate even the most remote corners of this rugged mountain country.
Reaching communities in far flung parts of this mountainous country is a logistical challenge, but one FPAN sees as crucial to its work. Teams of staff and volunteers spend days travelling by vehicle or, if necessary, on foot to make sure they reach people.
“Accessibility is a big challenge, especially in rainy season when the road gets blocked and our staff have to walk carrying all the devices,” says Devendra Amgaim, FPAN’s project coordinator in Rasuwa, northern Nepal.
“I go to remote places, where people and don’t know about family planning,” says Binu Koraila, an FPAN staffer in Rasuwa. Her role is spread knowledge about family planning and contraception among rural communities and to train the government workers who staff the health posts, many of which are many hours’ walk from the hamlets and villages that perch on the Langtang mountains.
Cultural beliefs
High up in the mountains of northern Nepal, close to the border with Tibet, lies the village of Gatlang. This cluster of timber-framed houses and Buddhist stupas is home to some of Nepal’s 1.5 million Tamang people, an ethnic group with cultural traditions stretching back centuries.
Life here is strictly patriarchal. Marriage often takes place young – from around 14 years old – and girls are given little choice about when or whom they will marry.
“My parents forced me to get married,” says 20-year-old Jomini.
Jomini married at the age of sixteen, to a man eight years her senior. “It’s not easy being married, it’s difficult,” she says. “When I got married, I didn’t know anything about what happens after marriage, about the physical side … and after the birth of my first child I had many difficulties.”

According to Nepali law, marriage under the age of 20 is illegal. But over 40% of 20 to 24 year olds are married before they turn 18. The effect on girls’ lives can be devastating: physical problems from teenage pregnancy, psychological trauma, thwarted education and employment opportunities are widespread, particularly in remote regions.
Access to contraception means nothing unless people understand why it is important and make the decision – armed with the correct information – to use it freely themselves.
Busting the myths that can shape people’s ideas about family planning is complex but vital. FPAN does it by spending time and resources on teams who go in and talk to women and families in ways that are tailored to their needs.

“Rasuwa district has a very low literacy rate, so FPAN … gives people the right information about family planning using visual aids, images and charts,” Devendra Amgaim explains. “Reproductive health female volunteers also translate information into local languages. All this helps make information simpler, more effective and easily understandable.”
The organisation strives to make sure it is sensitive to the structures that shape life in Rasuwa. This is also pragmatic: once you have won the trust and confidence of community leaders, it is much easier to talk to the rest of their community.
“FPAN seeks out the people who have influence in the communities – the religious leaders, the teachers, the female voluntary workers,” Devendra says. “We give them orientation and knowledge regarding those misconceptions. They then create awareness.”
Stories
Read more stories from Nepal
when
country
Nepal
Subject
Contraception, Comprehensive Sex Education, Gender equality, Maternal Healthcare, Emergencies
Related Member Association
Family Planning Association of Nepal