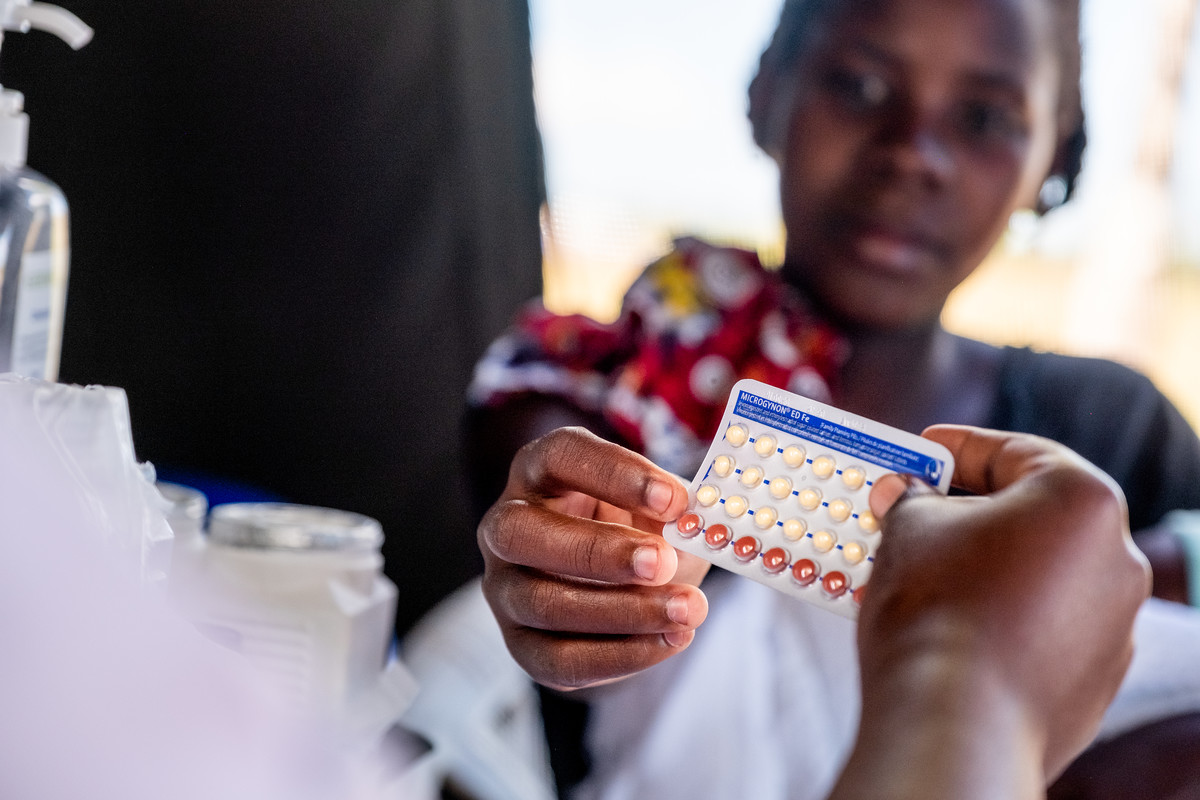
Globally, the unmet need for contraception remains too high. It’s estimated that 214 million women and girls are not using modern contraception, despite wanting to avoid pregnancy. And this was before the COVID-19 pandemic, which is set to further derail access to contraception for women and girls around the world.
Disrupted supply chains
Lockdown measures taken globally to respond to COVID-19 are bringing major disruptions to contraceptive supply chains. Large manufacturers of contraceptives in Asia have had to halt production or operate at reduced capacity, and we may see similar developments in other regions as COVID-19 takes hold.
For example, the world’s largest condom producer – Malaysia’s Karex Bhd – which makes one in every five condoms globally, was forced to close for a week in March and only given permission to reopen at 50% capacity. Production of IUDs in India – a major global producer of IUDs – has come to a standstill with the Indian government also curtailing export of any product containing progesterone, a key component of a number of contraceptives.
In addition to this, the closures of borders and other restrictions imposed in the face of COVID-19 further affect the shipping and distribution of commodities.
Delays in the production and delivery of contraceptive supplies at global and national levels will lead to stockouts of supplies, severely impacting contraceptive access.
Disrupted access
Beyond this, at country level, sexual and reproductive health services, staffing and funds may be diverted to support COVID-19 responses, leaving women and girls unable to access contraceptive and other sexual and reproductive health care. Provision of sexual and reproductive health services will also be affected by infection prevention measures, including health workers’ access to personal protective equipment (PPE).
Yet, this is just part of the picture. Even where contraceptives are available and continue to be provided through clinics or pharmacies, the impact of COVID-19 on women’s and girls’ lives will curtail their access in multiple other ways. Quarantine measures and mobility restrictions will affect women’s and girls’ ability to seek out contraceptive services. Financial insecurity and additional caregiving burdens brought on by lockdown measures will be further impediments. Marginalized populations will face additional barriers.
What’s the impact for our clinics on the ground?
In 2018, we delivered 81.2 million contraceptive services and distributed over 300 million condoms through our Member Associations (MAs). Contraceptive care, either through clinics or outreach programs, makes up the largest portion of our service provision to communities by far.
Now, in the face of the COVID-19 pandemic, we are receiving concerning updates from our MAs who are worried about impacts on supply chains and their ability to operate. 5,633 static and mobile clinics and community-based care outlets have already closed because of the outbreak, across 64 countries. They make up 14% of the total service delivery points IPPF members ran in 2018. For MAs that are still running limited services, an immediate need is PPE.
Where does this leave us?
At IPPF, supporting all our MAs through this pandemic is our priority. We are working to understand the stresses being placed on our MAs and to deliver as much direct support as possible. We actively monitor the impact of COVID-19 on the supply of contraceptives and other sexual and reproductive health commodities, and work with partners and manufacturers to do what we can to meet MAs’ needs – including for PPE – and ensure continued availability of supplies.
We are also working to identify opportunities to modernize our service offering to respond to the rapidly changing landscape, with a view to expanding no touch and digital services and self-management of care, and make a strong case for additional resourcing in these challenging times.
And we are calling on others – national governments, donors and international agencies – to recognize sexual and reproductive healthcare, including contraceptive services, as essential in this crisis, and to take measures to address disruptions in supply chains and ensure continued service provision at national level.
If women, girls and marginalized communities cannot access contraceptive care in this crisis, we can expect to see a rise in unintended and forced pregnancies, an increase in sexually transmitted infections, including HIV, and, ultimately, a sharp rise in unsafe abortions. The impacts on women’s and girls’ lives now, and beyond this crisis, will be severe.
when
Subject
Contraception