SIZE defines many things about Nigeria. Being Africa’s most populous country ensures that plenty of the issues it faces are big.
Nigeria’s population is around 188 million, and growing at more than 3% a year. Around a quarter of young women will be mothers or pregnant by the age of 19.
One reason is a historically low use of contraception – at around 10%. One estimate suggests 35% of 15-24-year-olds who want access to contraception can’t get it – creating a huge unmet need for family planning.
Nigeria’s Government has pledged to do something about that gap. It wants to increase the use of contraception to 36% by 2018 - its part in the global effort to give women around the world equal access to contraception.
And a pilot programme run in Oyo State by the Planned Parenthood Federation of Nigeria (PPFN), IPPF’s national member, has offered startling progress.
ClusterPLUS is something of a hybrid. It was built on the foundation of PPFN’s previous work but added new thinking, including ideas developed by IPPF member associations in Kenya and Uganda, who helped PPFN adapt them for Nigeria.
At its heart is a simple concept - partnership. The closer you can get to local communities, the better you work with national and local government and more you try to build local ownership, the better.
The project used PPFN’s earlier development of “clusters” of clinics, pharmacies and other outlets, as a base. The original cluster project, introduced in 2009, was funded in part by the UK Department for International Development.
One ClusterPLUS innovation was a tireless approach to community outreach. In villages without permanent centres, clinics would set-up for three days at a time in schools, churches, markets or mosques. But to make sure everyone who could benefit from them knew they were coming, workers armed with enthusiasm and megaphones would go around drumming-up interest first.
These CHEWS (Community Health Extension Workers), lent from Nigeria’s Ministry, did far more than generate publicity though.
They also lived in the communities and were trained to supply forms of contraception themselves. Women unable to get to a clinic, perhaps because of work, could visit a CHEW at home in the evening. Often they might bring a friend too. Greater accessibility boosted the numbers of women using contraception.
Sherifat Adelke is a 32-year-old CHEW with the Joy Hospital in Ibadan. She thinks her Islamic faith helped one fellow Muslim to end his opposition to his wife using contraception.
“He was furious at me and kept looking at my Hijab. Then he asked me if I was a Muslim at all. I told him the Quran didn’t instruct Muslims not to use Family Planning. After enough lecture, he agreed. That was a victory for me.”
Male opposition wasn’t anything new. PPFN was already using “male motivators” to combat men’s ignorance about contraception.
Owolabi Temidayo is one male motivator in Ibadan.
“Some men believe that when their wives start using family planning they will become promiscuous. Others believe if their wives have implants they won’t be able to enjoy intercourse. The religious ones believe family planning is a sin.
"I go places to educate men. I go to motor parks, markets, town hall meetings, speaking on the need for family planning. It goes a long way in clearing the misinformation out there.”
One partnership which proved critical to ClusterPLUS was between PPFN and local government in Oyo State – it helped to galvanise local leadership and create buy-in from officials.
And the support was concrete. As well as providing three clinical staff, local authorities supplied the contraceptives and places for training, for meetings and for clinics.
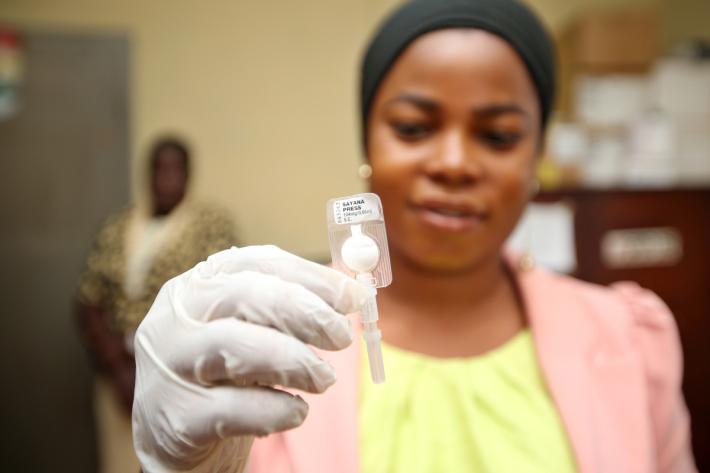
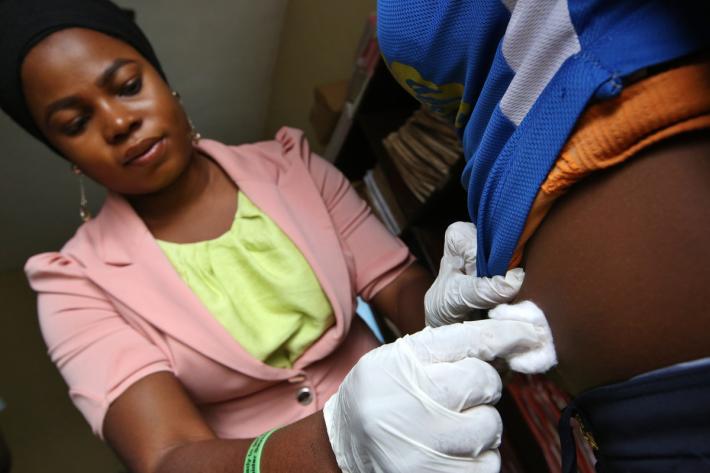
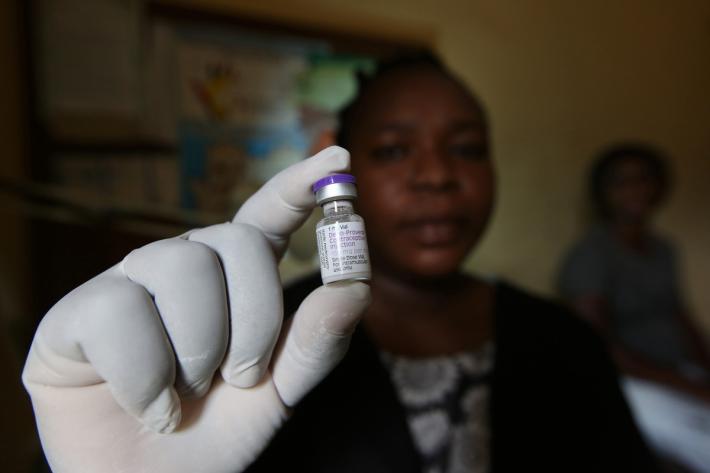
ClusterPLUS also set out to emphasize the benefit of long acting forms of contraception such as implants and IUCDs. And their provision was integrated with other services. Someone coming to a clinic for breast or cervical cancer screening or a test for HIV or a sexual transmitted infection would find family planning available there and then.
Reaching those in poorer communities was also a priority. 28-year-old Tawa Agungbaide was responsible for making sure that one group of 63 women who couldn’t afford to pay for contraception gain access to it nevertheless.
“We realized finance was a huge challenge. In some instances, it wasn’t a question of paying for services, but also of not even having enough money to pay for their transport to a clinic.”
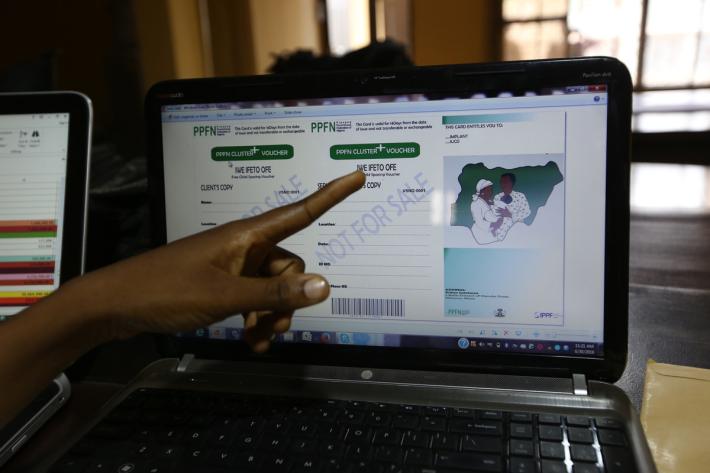
The solution, says Tawa, was a voucher scheme, funding transport and contraception for women who simply couldn’t fund it themselves. It helped her group and many others.
“With eligibility criteria, we were able to single women who really couldn’t afford family planning. The voucher scheme was able to solve that. I feel fulfilled helping these women.”
And new technology has played a major part too. An app on tablets and smartphones allowed health workers to input what they’d handed out every day – quickly and in real time. The supply team could then make sure that a delivery point never ran out of supplies – avoiding the dreaded stock-out.
How well has it worked? The figures are impressive. The project aimed to reach 20,200 people in its nine months. It actually got to 53,152 clients.
But as well as reaching more people, with more family planning services, it also gave women wider choice about the form of contraception they wanted. Two thirds of new users chose long-acting forms of contraception, more than double the rate outside of the project.
The aim for PPFN now is to roll out the same approach across Nigeria, reaching more young people, especially poorer women. ClusterPLUS is already running in three other states in Nigeria – and if it proves as successful as in Oyo State, Nigeria’s Government will be making big progress towards its family planning pledge.
when
country
Nigeria
Blog Series
Adolescent Health
Subject
Contraception, Maternal Healthcare, Gynaecological
Related Member Association
Planned Parenthood Federation of Nigeria