“All I do is sit and cry with my children. I want family planning so bad. I’ve known about it, but I have never managed to get it,” says Esther, 31, sitting in the tiny village on the island of Ambae, in Vanuatu. On her lap is her youngest child, Elijah.
Next to her on the mat is her two-year-old child, Stewart. Running around outside her modest house are her four other children - George, 12, James, 10, Steven, 8, and Judith, 6.
Esther lives on the Manaro Voui volcano in Vanuatu - where sudden recent seismic activity causes it to belch toxic fumes. Esther’s husband is barely home. Her second youngest, Stewart, has a disability and cannot walk. Her youngest, Elijah, was born one week before the family were forced to evacuate to another island.
Entire island evacuated
On her own, Esther packed up their home and safely brought her children to the evacuation centre. This was the first time that an entire island population had been evacuated in the Pacific Region.
Once the threat level was decreased and the population returned, the Vanuatu Family Health Association, through the International Planned Parenthood Federation, commenced a humanitarian response with mobile health clinics and awareness sessions.
The services available through the clinics included pregnancy and delivery support, contraceptives such as condoms, injectables, implants and emergency contraceptives, and screening and management of sexually transmitted infections.
Often the communities were in areas that were impassable by road, so the VHFA response team - which included nurses and midwives - travelled by boat and foot with their medical supplies to reach those closest to the crater. Esther lived in one of those villages, evident by the smoke constantly billowing out of the crater in the near distance.
Raising six children alone was already difficult for Esther but her life was made even harder during and after the evacuation. Emergency situations are particularly unsafe for women and children, who are more likely to die during an emergency than men. Transmission rates of sexually transmitted infections - including HIV - increase during an emergency, as does sexual violence and maternal deaths.
Esther desperately wanted access to long term contraceptives. The nearest clinic for her is a two-hour way away, almost impossible with six children in tow. When the Vanuatu Family Health Association arrived at her village they were able to counsel her about her contraceptive options, and return the following week to give Esther a five-year contraceptive implant.
Increased sexual literacy
‘Mothers do everything in Vanuatu, so having a smaller family makes it easier to move around in emergencies,’ says Julie Aru, a nurse working with VHFA during their humanitarian response. This is particularly important in Vanuatu, which according to the World Risk Index, is the most disaster-prone country in the world.
‘But the biggest issue is isolation. Mothers do not have access to family planning even in stable times,” says Julie. “The second issue is ‘kastom’ - religious and cultural beliefs – which sometimes don’t allow women access to family planning. We are working to change this.”
Whilst emergencies create immense challenges, they also provide opportunities for organisations like the Vanuatu Family Health Association to reach remote communities such as Esther’s, to increase sexual literary rates, and to provide women with reproductive choices. By the end of the response, VHFA had reached over 1,600 people across the southern part of Ambae Island with sexual and reproductive health care and information, and 480 dignity kits were distributed on North and East Ambae.
when
country
Vanuatu
Subject
Emergencies
Related Member Association
Vanuatu Family Health Association















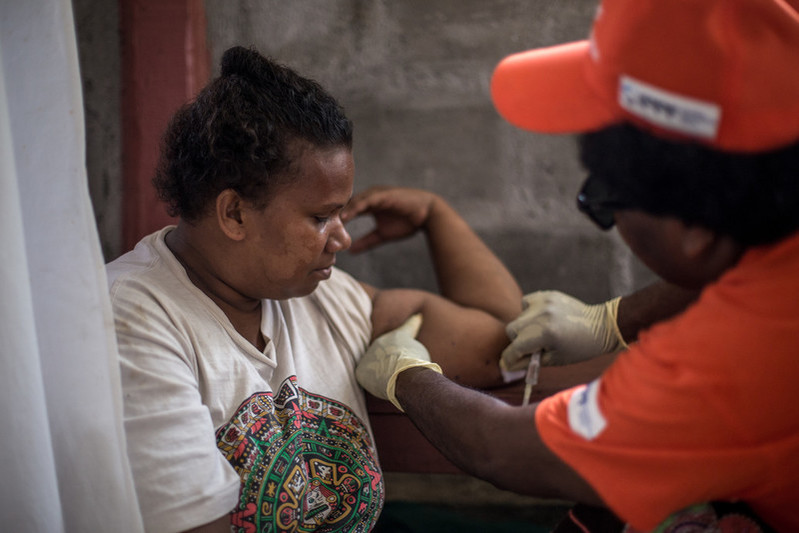



![Natalie is seven months pregnant. She lives with her son Johnson high up on the volcano's steep sides. The mobile outreach team visited her village and give vaccinations to her son. "When the volcano started to become active, we could hear the noise of the volcano erupting and see the smoke in the sky. We had to walk down the mountain to Lone, it took many hours," says Natalie. "After I deliver this child I want to get the ‘five-year stick’ [Jadelle]. It will make life easier.”](/sites/default/files/slideshows/IPPF%20Humanitarian%20-%20Vanuatu%20Volcano%202017_60095_IPPF_Kathleen%20Prior_Vanuatu_IPPF%20.jpg)









