Christine Latim is a 45-year-old grandmother is living with HIV. She has been on antiretroviral treatment since 2005 and was widowed in 2006. She thinks her husband died of an HIV-related infection.
“I heard on the radio that for people living positively it was a serious risk for us to get cervical cancer. During the announcements they mentioned some of the signs of cervical cancer like bad smell and so many signs.
“I was having signs of discharge and very bad smell,” she said.
She needed a smear to check for cervical cancer but getting one in rural Uganda wasn’t easy because money was tight and there were few gynaecologists available.
“I tried in TASO Uganda, I failed. I went to Lachor Hospital, I never got satisfied.
“Early in 2013, I heard over the radio about the services being offered by Reproductive Health Uganda. I went to their service centre and I was examined for cervical cancer and I tested positive. I got services from that centre. Last August, when I went for my control, they found that I’m free of cervical cancer” said Latim.
When she went for the smear for cervical cancer at Gulu Clinic she was also tested for human papilloma virus (HPV).
Today Christine is visited by two people at her thatched hut home four kilometres away from Gulu Clinic. It is part of the routine follow-up for patients.
From first appearance, it is hard to believe that this grandmother of one is living with HIV until she tells you that she is living positively. In her hut, the portrait of her late husband is displayed on the wall.
Smartly dressed in a white and black coloured long dress, Latim said she had seen many friends that had died of cervical cancer.
“Gulu Clinic has changed my life completely because of the way they handle their clients. And we got the service at a lower cost than at other health centres.
“If I had any capacity to talk to government or any non-governmental body, I would say they should support RHU Uganda for their good service to youth, women and those of us that are positive living” said Latim.
Latim’s prayer is that Gulu Clinic scales up more services targeting the youth in her community.
“In our country if the youth is healthy many of our youth have experienced a long period of conflict so they need more sensitization especially for their health.” she added.
Follow a day in the life of our team and clients in Gulu, Uganda
-
7am: The team prepare for the long day ahead

"Every year tens of thousands of Ugandans come to our clinic. Everyone is welcome. Here are just a few of the people that we served in one day last month."
-
8am: Nancy, 19, becomes a volunteer

"I was suffering but when I came here, I was treated and I got better. Now I'm inspired to volunteer here"
-
9am: Monica, 25, a sex worker's story

"I am sex working. I came here for Hepatitis B testing and also counselling. I have so many personal problems, but here….they’re so caring."
-
10am: Jane, 23, saved by family planning
"After multiple miscarriages, family planning here has helped me a lot. I'm glad we've been able to space the number of children we've had. I am not growing old, I am fresh."
-
11am: Vicky, handling disabilities

"I'm deaf so accessing services is hard, but here they really try to speak in sign language."
-
12pm: Dorcus, first time patient

"This is the first time I've ever come here, I like the service. They give good counselling so I recommend coming."
-
1pm: Christine, 45, a grandmother's tale of living with HIV

"I am living with HIV and had HPV. They treated me and now I'm free of cervical cancer."
-
2pm: Lilian, struggling mother of six with sickle cell

" I have sickle cell disease and so do all my children. I want to have my tube removed so that I don't get pregnant again but I don't know if my husband will allow it."
-
3pm: Brenda and Francis get fertility treatments

"Fertility treatment is a sensitive issue in Uganda but they help us a lot and we get proper treatment."
-
4pm: Joyce, 25, repected regardless of her disability
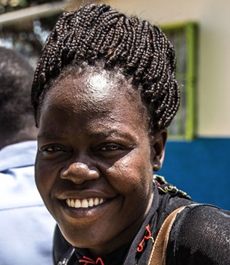
"I realised that at this place they don't segregate. Us people with disabilities have challenges at the main hospitals. You go there, people around look at you as if you are not a human being and you don't fall sick."
-
5pm: Mobile clinic provides outreach services to remote villages

"Our outreach to remote communities is a 'one-stop-centre'. We give family planning, vaccines for HPV, malaria, and Hepatitis B, HIV testing and more."
-
22pm: Still giving the last client our very best
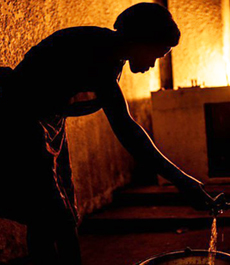
"Together, we have great teamwork. Sometimes we're still working up to 10pm because we never chase out our clients. We’ll never close the place when we have a client inside. People come when they have no hope."
when
country
Uganda
Subject
HIV and STIs, Gynaecological
Related Member Association
Reproductive Health Uganda








