Every Thursday a team from RHU Gulu district provides a mobile outreach clinic in Atega village in the Omoro district in Northern Uganda. The outreach team goes out into this poor, remote area which would otherwise not have access to sexual and reproductive health services.
The night before the outreach clinic RHU driver, Robert Nyeko and Godfrey Bedimot load up tents, chairs, medical equipment and supplies. The clinic needs to be set up and by 7am ready to receive clients from 8am.
The outreach clinic provides a range of services including diagnosis, testing and treatment, family planning such as fitting implants, providing condoms and HPV vaccines. Laboratory technician, Denis Bongonyinge carries out testing for malaria, Hepatitis B, HIV/AIDS, pneumonia and other infections. Other members of the team provide immunisations and vaccinations.
Typically men, women and children start arriving at the clinic by 7:30am. Two volunteers are on hand to direct them to the appropriate place to get the services they need. Some clients need a range of services.
At 8am service provider, Anicia Filda, popularly known a 'Mama' in the community is ready with her team to start the day. There are now more than 200 clients waiting to be seen; with more people arriving to join the long queues.
The longest queue is for the immunisation and vaccination services. The majority have come for either the Hepatitis B vaccine, which is a big threat in this community. Priority is given to the many young girls lining up for the Human Papilloma Virus (HPV) vaccine.
Denis Bongonyinge takes blood samples for rapid tests for malaria, HIV, HPV and a range of other infections. Each client carries an exercise book where Denis records their results which is then taken to the staff giving out prescriptions.
32-year-Robert Otim pushes his bicycle to the outreach clinic. The single father has ridden 10 kilometres with his two young children. He lost his wife to Hepatitis B when their daughter was just six months. His four-year-old son was born prematurely and is now disabled. He has come today for his last Hepatitis B immunisation. His children need to be vaccinated as well as treated for malaria and coughs. Looking at the long queue, he says he doubts whether he will get the service today but he is lucky as one of the team who once treated his son, Geoffrey, notices Robert and they are given priority for treatment and prescriptions.
Already by midday, one of the teams delivering minor surgeries, postnatal services, family planning and post abortion care have seen 47 mothers. This is almost the same as the number of clients they would treat at the Gulu Clinic during a normal day.
Anicia Filda sends the driver to collect more supplies from the clinic; the stock is starting to run low because demand is so high There is no break for the team. Samuel Kedi, the only clinician at the outreach camp stands up, and picks up a bottle of water from his backpack for a quick drink before continuing with the next client.
The clinic continues to see clients well into the evening. The outreach clinic is scheduled to finish by 5pm but Anicia says there is not one day they have closed on time: “We cannot close when clients are still lining up. It’s the same at the clinic in Gulu,” she says.
As the clinic draws to a close for the day, the teams complete their report which records details of the numbers clients served, the types of services delivered and supplies of stock. It has been another busy but successful day for Anicia and her team. Provision of integrated services in such remote areas is vital for the local community; many men, women and children would not be able to receive the types of treatment and care that RHU works diligently to provide.
Follow a day in the life of our team and clients in Gulu, Uganda
-
7am: The team prepare for the long day ahead

"Every year tens of thousands of Ugandans come to our clinic. Everyone is welcome. Here are just a few of the people that we served in one day last month."
-
8am: Nancy, 19, becomes a volunteer

"I was suffering but when I came here, I was treated and I got better. Now I'm inspired to volunteer here"
-
9am: Monica, 25, a sex worker's story

"I am sex working. I came here for Hepatitis B testing and also counselling. I have so many personal problems, but here….they’re so caring."
-
10am: Jane, 23, saved by family planning
"After multiple miscarriages, family planning here has helped me a lot. I'm glad we've been able to space the number of children we've had. I am not growing old, I am fresh."
-
11am: Vicky, handling disabilities

"I'm deaf so accessing services is hard, but here they really try to speak in sign language."
-
12pm: Dorcus, first time patient

"This is the first time I've ever come here, I like the service. They give good counselling so I recommend coming."
-
1pm: Christine, 45, a grandmother's tale of living with HIV

"I am living with HIV and had HPV. They treated me and now I'm free of cervical cancer."
-
2pm: Lilian, struggling mother of six with sickle cell

" I have sickle cell disease and so do all my children. I want to have my tube removed so that I don't get pregnant again but I don't know if my husband will allow it."
-
3pm: Brenda and Francis get fertility treatments

"Fertility treatment is a sensitive issue in Uganda but they help us a lot and we get proper treatment."
-
4pm: Joyce, 25, repected regardless of her disability
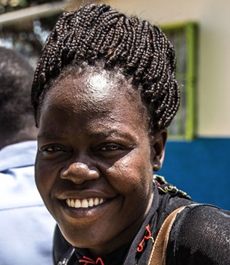
"I realised that at this place they don't segregate. Us people with disabilities have challenges at the main hospitals. You go there, people around look at you as if you are not a human being and you don't fall sick."
-
5pm: Mobile clinic provides outreach services to remote villages

"Our outreach to remote communities is a 'one-stop-centre'. We give family planning, vaccines for HPV, malaria, and Hepatitis B, HIV testing and more."
-
22pm: Still giving the last client our very best
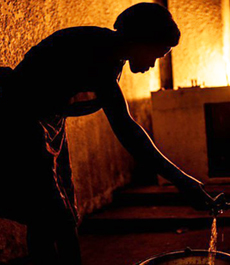
"Together, we have great teamwork. Sometimes we're still working up to 10pm because we never chase out our clients. We’ll never close the place when we have a client inside. People come when they have no hope."
when
country
Uganda
Subject
Contraception, HIV and STIs, Maternal Healthcare, Gynaecological
Related Member Association
Reproductive Health Uganda











