
Uganda has one of the highest fertility rates in the world, and as a result, it also has one of the most youthful populations - more than half of Ugandans are under the age of 15. Over 78% of the population is below the age of 30.
The population is growing at a rate of more than 3% per year. Figures show that women – on average - give birth to two more children than they want.
More than half of pregnancies in Uganda are unintended, and nearly a third of these end in abortion according to figures from the Guttmacher Institute.
It also says that in Uganda approximately one in every 19 women has an abortion per year and with abortion being highly restricted most of these are unsafe. This rate is far higher than the average for East Africa and reflects the high level of unmet need for contraception in the country.
Approximately, 755,000 unintended pregnancies occur annually out of which 297,000 result in unsafe abortions.
Unintended pregnancy is common in Uganda, leading to high levels of unplanned births, unsafe abortions, and maternal injury and death. Women in the eastern and north regions had the highest proportions of unplanned births (50–54%) the high levels of unintended pregnancy and unplanned births in Uganda can be attributed primarily to nonuse of contraceptives by women who do not want a child soon.
More than 80% of the population lives in rural areas. Millions of people still do not have access to a health clinic, and family planning, especially long term and permanent methods, is not available to the vast majority who live in rural and hard-to-reach areas.
IPPF’s Member Association, Reproductive Health Uganda (RHU), is working hard on the ground to tackle these issues. It takes the approach that it offers people as many services as possible at its clinics so you can get your health needs met in the same place.
This means you might go to a clinic for an HIV test but leave having being offered a range of contraception plus other tests for other sexually transmitted diseases or cancer.
RHU has a network of clinics across the country and takes its services out to remote and rural areas through its mobile clinics. No one is left out by RHU. Whether people are poor or vulnerable or hard to reach, RHU makes sure they have access to all of the services they need.
We visited one of RHU’s health facilities in northern Uganda to get a better idea of how our work makes a real difference to people and their lives. We wanted to hear stories about what difference getting contraception, counselling and testing meant in reality. For many people it is life-changing.

Thousands of people go in and out of Gulu Clinic every year and thousands more get services through Gulu’s mobile clinics. Last year alone Gulu Clinic had 229,812 family planning clients and provided 769,707 sexual health services, 390,488 of those were to young people.
It offers a ‘one-stop-shop’ approach which makes it easier for clients to get a range of integrated services. They can go to a clinic for a check-up but end up getting contraception, counselling and a whole range of other tests and treatments.
These include family planning, infertility management, cervical cancer screening, cryotherapy, youth friendly services, sexually transmitted infections and general sexual and reproductive health (SRH).
Denis Bongonyinge, who has worked at Gulu Clinic for four years, said: “For us our goal is to ensure that this place is just a one stop centre. When a client comes in, he goes out when he has got a very big package of services within the clinic. Even if we go out, we give very many services.
Denis said he had come across a range of issues among the clients. Issues like high rates of teenage pregnancies, sexually transmitted infections and gender based violence which could all be dealt with at the centre.

He added that he believed Gulu had managed to offer such a range of services because of its willingness to work with other partners interested in scaling up uptake of family planning and generally sexual and reproductive health services.
Gulu Clinic is also inclusive to a wide range of people across the community and this includes sex workers and disabled people.
Vicky Acora is deaf and has had problems getting services at other hospitals.
But, she says about RHU: “They are really most welcoming and they try to communicate even in the little sign language they know. They are really very warm”
She says she has since been advising other deaf persons to seek services at Reproductive Health Uganda because of the quick services.
“I encourage other people to come here because it is fairer. I encourage other disabled people who use wheelchairs not only the deaf to come and access services here because it is really accessible for those who have a disability.”
Follow a day in the life of our team and clients in Gulu, Uganda
-
7am: The team prepare for the long day ahead

"Every year tens of thousands of Ugandans come to our clinic. Everyone is welcome. Here are just a few of the people that we served in one day last month."
-
8am: Nancy, 19, becomes a volunteer

"I was suffering but when I came here, I was treated and I got better. Now I'm inspired to volunteer here"
-
9am: Monica, 25, a sex worker's story

"I am sex working. I came here for Hepatitis B testing and also counselling. I have so many personal problems, but here….they’re so caring."
-
10am: Jane, 23, saved by family planning
"After multiple miscarriages, family planning here has helped me a lot. I'm glad we've been able to space the number of children we've had. I am not growing old, I am fresh."
-
11am: Vicky, handling disabilities

"I'm deaf so accessing services is hard, but here they really try to speak in sign language."
-
12pm: Dorcus, first time patient

"This is the first time I've ever come here, I like the service. They give good counselling so I recommend coming."
-
1pm: Christine, 45, a grandmother's tale of living with HIV

"I am living with HIV and had HPV. They treated me and now I'm free of cervical cancer."
-
2pm: Lilian, struggling mother of six with sickle cell

" I have sickle cell disease and so do all my children. I want to have my tube removed so that I don't get pregnant again but I don't know if my husband will allow it."
-
3pm: Brenda and Francis get fertility treatments

"Fertility treatment is a sensitive issue in Uganda but they help us a lot and we get proper treatment."
-
4pm: Joyce, 25, repected regardless of her disability
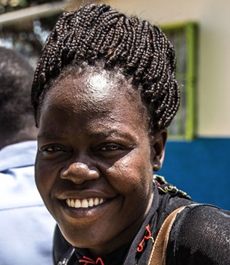
"I realised that at this place they don't segregate. Us people with disabilities have challenges at the main hospitals. You go there, people around look at you as if you are not a human being and you don't fall sick."
-
5pm: Mobile clinic provides outreach services to remote villages

"Our outreach to remote communities is a 'one-stop-centre'. We give family planning, vaccines for HPV, malaria, and Hepatitis B, HIV testing and more."
-
22pm: Still giving the last client our very best
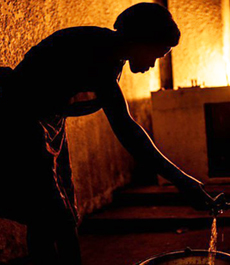
"Together, we have great teamwork. Sometimes we're still working up to 10pm because we never chase out our clients. We’ll never close the place when we have a client inside. People come when they have no hope."
when
country
Uganda
Subject
Contraception, HIV and STIs, Abortion Care, Maternal Healthcare, Gynaecological
Related Member Association
Reproductive Health Uganda








